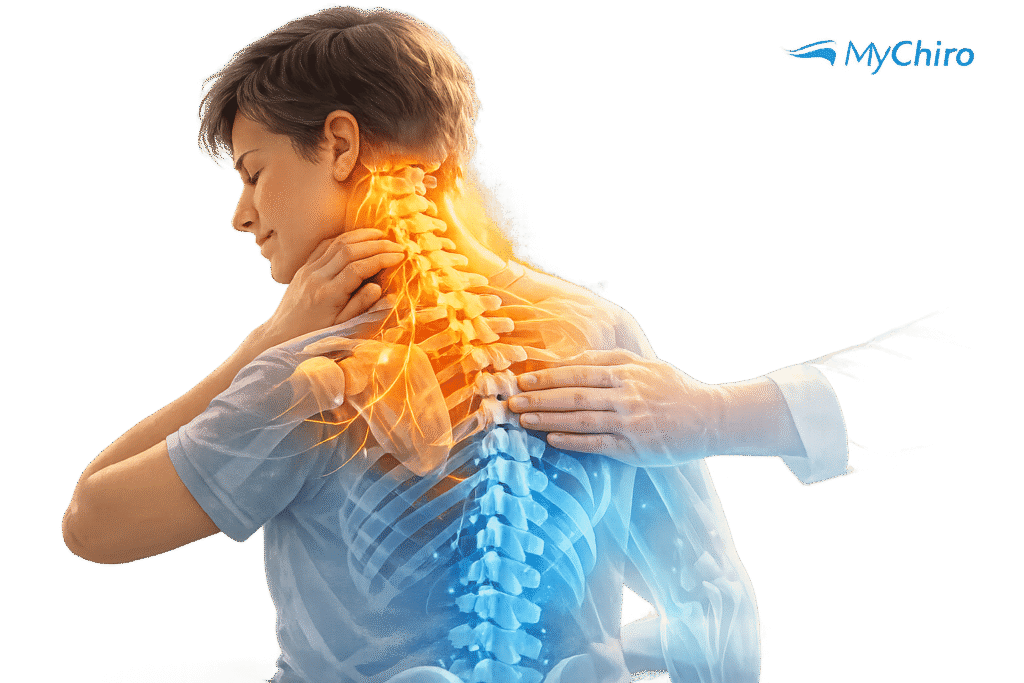
Stress can change how your nervous system processes pain, making even mild discomfort feel worse. When stress is chronic, it can disrupt your body’s hormonal balance, heighten inflammation, and increase sensitivity to pain. This is often linked to conditions like fibromyalgia and chronic fatigue syndrome. Your brain and spinal cord may also become overly reactive, amplifying pain signals – a process called central sensitisation.
Key points include:
- Chronic stress disrupts the HPA axis, leading to hormonal imbalances like high or low cortisol levels.
- Stress rewires the brain’s "pain matrix", making it harder to manage pain and emotions.
- Muscle tension in areas like the neck and shoulders is a common physical result of stress.
- Chiropractic care may help reduce muscle strain, improve spinal alignment, and support the nervous system’s shift from "fight or flight" to "rest and recover."
Addressing stress and pain involves combining physical care, like chiropractic adjustments, with lifestyle changes such as better posture, regular exercise, and mindfulness. Together, these approaches can help manage the effects of stress on your body and mind.
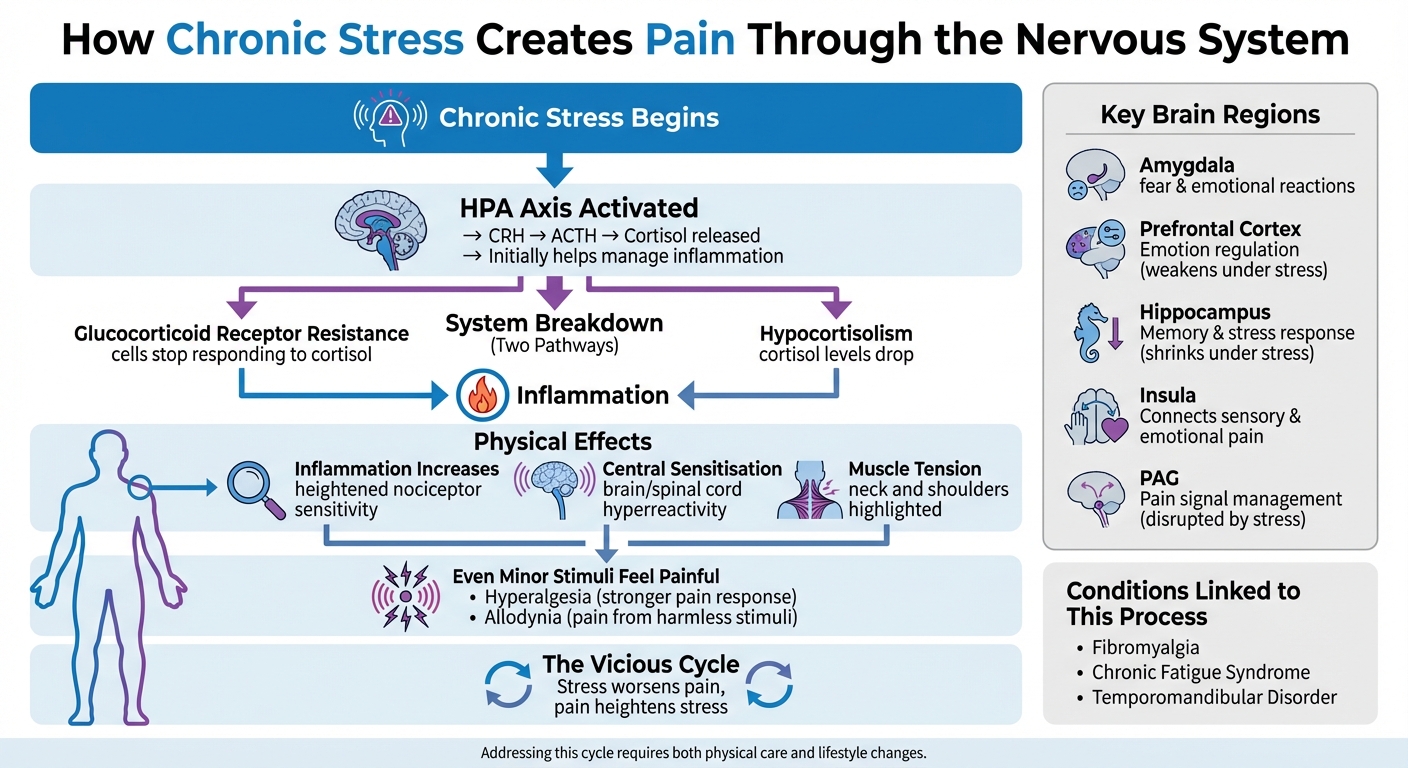
How Chronic Stress Creates Pain Through the Nervous System
How to treat Chronic Pain in the Brain, Body, and Nervous System
How Stress Affects the Nervous System and Creates Pain
When stress becomes chronic, it activates the HPA axis (hypothalamic-pituitary-adrenal axis), triggering the release of CRH, ACTH, and cortisol. Initially, this process helps manage inflammation, but over time, the system can break down. Prolonged stress can lead to two distinct issues: glucocorticoid receptor resistance (where cells stop responding to cortisol) or hypocortisolism (a drop in cortisol levels after extended stress). These hormonal imbalances are linked to conditions like fibromyalgia, chronic fatigue syndrome, and temporomandibular disorder. Such changes in cortisol regulation can fuel inflammation, which, in turn, amplifies pain sensitivity.
HPA Axis Dysfunction and Chronic Pain
When cortisol’s regulatory role falters, inflammation runs unchecked. This can damage tissues and heighten the sensitivity of nociceptors – the nerve endings that detect pain. The result? Even minor physical stimuli can feel intensely painful.
"The HPA axis may be in the state of hyperactivity at the early stage of pain chronification, while, after long-term overt activity, the stress system reaches an exhausted state, thereby turning into the HPA axis hypoactivity." – Xiaoyun Li and Li Hu, Southwest University
Chronic stress keeps cortisol levels elevated for extended periods, disrupting the natural feedback loop that controls hormone release. This creates a vicious cycle: stress worsens pain, and pain heightens stress. Over time, this ongoing stress not only drives inflammation but also rewires neural pathways, leading to a heightened sensitivity to pain.
Central Sensitisation from Repeated Stress
Stress doesn’t just impact hormones – it can fundamentally alter how the nervous system operates. This process, known as central sensitisation, keeps the brain and spinal cord in a state of heightened reactivity, making normal sensations feel painful.
Chronic stress can increase NMDA receptor activity and glutamate levels, particularly in the amygdala, which processes fear-based memories. This lowers the pain threshold, leading to hyperalgesia (stronger pain from typically mild stimuli) and allodynia (pain from stimuli that should be harmless). Additionally, persistent stress can maintain elevated tension in muscles, especially in the neck and shoulders, further contributing to chronic discomfort.
Brain Networks That Connect Stress and Pain
Stress and pain are closely linked through brain networks that can intensify one another. Prolonged stress can alter the nervous system, creating a cycle that makes both stress and pain harder to manage. Key brain regions involved include the amygdala (handling fear and emotional reactions), the prefrontal cortex (managing emotions and decision-making), the insula (connecting sensory input with emotional pain), and the hippocampus (controlling memory and the stress response). Together, these areas form the "pain matrix." When chronic stress disrupts their roles, it can lead to persistent discomfort.
The amygdala acts like an alarm, spotting threats and activating the HPA axis to release cortisol. Under chronic stress, this "alarm" becomes overly sensitive, amplifying pain signals and fear. Normally, the prefrontal cortex steps in to regulate these responses, but prolonged stress weakens this control. Similarly, the hippocampus, which helps shut down the stress response, can shrink due to ongoing stress, further reducing the brain’s ability to manage both pain and stress.
Key Brain Structures in Stress and Pain Processing
The pain matrix is divided into two main systems. The median matrix (including the anterior cingulate cortex, prefrontal cortex, and anterior insula) focuses on the emotional aspects of pain. The lateral matrix (involving the somatosensory cortices, posterior insula, and thalamus) processes physical details, like where pain is felt and how intense it is. Chronic stress can disrupt both systems, making pain feel more overwhelming and harder to ignore.
The periaqueductal grey (PAG) plays a vital role in managing pain signals. It connects higher brain areas to the spinal cord and normally helps suppress pain. However, with chronic stress, this system can shift, amplifying pain signals instead of calming them.
Short-Term vs. Long-Term Stress Effects on the Brain
Short-term stress is part of the body’s survival toolkit. When faced with immediate threats, the sympathetic nervous system and HPA axis kick in, releasing hormones like cortisol that can temporarily dull pain. This response happens quickly, with cortisol levels rising within about 15 minutes to help the body manage "fight or flight" situations.
But when stress becomes chronic, it takes a toll. The HPA axis can become overworked, leading to lower cortisol levels (known as hypocortisolism) and increased inflammation. Neuroimaging studies show that chronic pain is linked to reduced grey matter in the amygdala, prefrontal cortex, and hippocampus. This loss weakens the brain’s ability to manage stress and pain, creating a vicious cycle. As the prefrontal cortex loses control, the amygdala becomes more reactive, and the hippocampus struggles to shut down the stress response, leaving the brain stuck in a state of heightened sensitivity.
sbb-itb-585d67d
How Chiropractic Care May Help Regulate the Nervous System
Chronic stress often shows up in the body as muscle tension, poor posture, and discomfort. These physical symptoms are closely tied to hormonal and neural processes like HPA axis dysfunction and central sensitisation. Chiropractic care targets these musculoskeletal effects by focusing on the spine and surrounding tissues, potentially helping to ease the strain on an overworked nervous system.
Improving Spinal Alignment and Reducing Physical Tension
Studies reveal that people under high stress often have increased electromyographic (EMG) activity in postural muscles, such as the neck and shoulders, even when they’re at rest. This means their muscles remain partially contracted, leading to persistent tension and fatigue.
Chiropractic adjustments aim to improve spinal movement and alignment, which may decrease the mechanical stress on the spine. Research also indicates that better spinal alignment through these adjustments can reduce the frequency and intensity of pain signals. Pairing these adjustments with moderate physical activity and simple changes to your workspace – like adjusting monitor height or chair positioning – can further alleviate stress-related muscle tension.
These adjustments do more than just relieve localised tension; they may also play a role in balancing overall nervous system activity.
Calming an Overactive Nervous System
When the sympathetic nervous system is overactive, the body remains stuck in "fight or flight" mode, keeping muscles tense and pain sensitivity heightened. Chiropractic care may encourage a shift toward the parasympathetic "rest and recover" state by easing physical tension and improving spinal function.
Interestingly, research suggests that spinal manipulation may send somatosensory signals to the hypothalamus via the spinohypothalamic tract, potentially influencing how the brain handles stress responses. There’s evidence to suggest that chiropractic care can help address the physical effects of prolonged stress as part of a broader, multidisciplinary approach.
Combining chiropractic adjustments with breathing exercises and regular movement breaks may further assist the nervous system in transitioning from a heightened state to a more relaxed one. This holistic approach acknowledges that managing chronic stress and pain involves addressing both the physical and regulatory aspects of nervous system health.
Conclusion
Chronic stress doesn’t just impact your mood – it can actually change how your nervous system processes pain. Through mechanisms like HPA axis dysfunction, central sensitisation, and increased sympathetic activity, long-term stress can transform short-term discomfort into ongoing pain that interferes with everyday life. Understanding these processes sheds light on ways to find relief.
Managing nervous system activity involves more than simple tweaks. Chiropractic care might play a role in addressing the musculoskeletal effects of nervous system stress. By improving spinal alignment, easing muscle tension, and encouraging a shift from "fight-or-flight" to "rest-and-recover", chiropractic care could help bring balance. Pairing this with lifestyle changes – such as regular exercise, mindfulness, ergonomic adjustments, and better sleep habits – creates a more rounded approach to tackling stress and pain.
Chronic pain also carries considerable challenges for healthcare systems and economies worldwide, underscoring the importance of effective solutions. By addressing both the physical and regulatory aspects of your nervous system, you can take steps toward reclaiming your well-being.
If you’re dealing with ongoing tension or stress-related discomfort, consider a strategy that blends professional care with lifestyle adjustments. Chiropractor Dr Steve in Bondi Junction provides nervous-system-focused chiropractic care aimed at helping busy professionals, active parents, and wellness enthusiasts manage musculoskeletal stress in a natural and practical way – complementing the strategies explored in this article.
This information is general in nature and should not replace professional medical advice. Chiropractic care focuses on musculoskeletal health, and outcomes vary between individuals. Always consult a qualified healthcare professional before making health-related decisions.
FAQs
How can I tell if stress is worsening my pain?
Stress can amplify pain by tightening muscles and heightening sensitivity, often driven by hormones like cortisol. You might notice pain worsening during stressful times, along with signs like tension, fatigue, or trouble unwinding. Symptoms such as headaches, stiff muscles, or shifts in posture could also signal that stress is playing a role. Recognising these patterns and seeking advice from a healthcare professional can be key to managing the link between stress and pain effectively.
What is central sensitisation in plain English?
Central sensitisation happens when the nervous system becomes overly reactive to pain signals, leading to an increased perception of pain, even when there’s no active tissue damage. This phenomenon is often associated with chronic pain conditions, causing the body to respond more intensely to minor triggers or sensations.
Can chiropractic care help with stress-related muscle tension?
Chiropractic care can play a role in addressing muscle tension linked to stress by concentrating on the health of the nervous system and spine. Through gentle adjustments, it may help promote relaxation and restore balance in the body, potentially easing the tension that stress often brings.