Functional movement assessments help identify and manage ataxic gait, a walking pattern often linked to neurological issues like cerebellar disorders or sensory dysfunctions. These assessments break down movements into measurable parts, enabling healthcare providers to diagnose coordination problems and monitor progress over time. Key tools include:
- SARA (Scale for the Assessment and Rating of Ataxia): Evaluates motor functions like gait, balance, and limb coordination.
- Heel-to-Shin Test: Highlights lower limb coordination issues, such as difficulty judging distances.
- Tandem Gait Test: Assesses balance by requiring heel-to-toe walking in a straight line.
Abnormal Coordination Exam ; Tandem Gait
sbb-itb-585d67d
Main Functional Movement Assessments for Ataxic Gait
Clinicians rely on several specialised tools to assess the movement difficulties linked to ataxic gait. These tools help measure coordination issues and their severity, providing valuable insights for diagnosis and tracking progress. Here are three key assessments used to evaluate ataxic gait.
Scale for the Assessment and Rating of Ataxia (SARA)
The SARA tool measures the severity of ataxia by evaluating eight specific motor functions, including gait, stance, sitting balance, speech, and limb coordination. This comprehensive approach helps clinicians gain a clear picture of motor control challenges.
"At the bedside, clinicians use pattern recognition rather than any objective measurement… the bedside assessment of patterns is formalised by clinical scales, eg Scale for the Assessment and Rating of Ataxia (SARA)." – Journal of NeuroEngineering and Rehabilitation
SARA is particularly useful for monitoring conditions like Friedreich’s ataxia, spinocerebellar ataxias, ataxia telangiectasia, and brain tumours. Its subscores for gait, sitting, and tandem walking make it an effective tool for tracking changes in coordination over time.
Heel-to-Shin Test
The Heel-to-Shin Test examines lower limb coordination. The patient places their heel on the opposite knee and slides it down the shin to the ankle before returning to the starting point. Though this movement seems simple, it can highlight cerebellar control issues.
Clinicians watch for signs of dysmetria – difficulty judging distances. This may appear as the heel slipping off the shin, overshooting, or failing to reach the knee or ankle accurately. In one study of 70 participants (39 with ataxia), automated sensors measuring linear acceleration showed a strong correlation (0.7821) with expert clinical assessments, supporting the test’s reliability.
Tandem Gait Test
The Tandem Gait Test requires walking in a straight line, heel-to-toe, which narrows the base of support and challenges cerebellar balance systems. This test is a vital part of the SARA scale and can expose subtle coordination problems that might not show up during regular walking. By narrowing the margin for error, this test provides a clearer picture of balance and stability issues that affect daily activities.
Organic vs Functional Ataxic Gait: Understanding the Differences
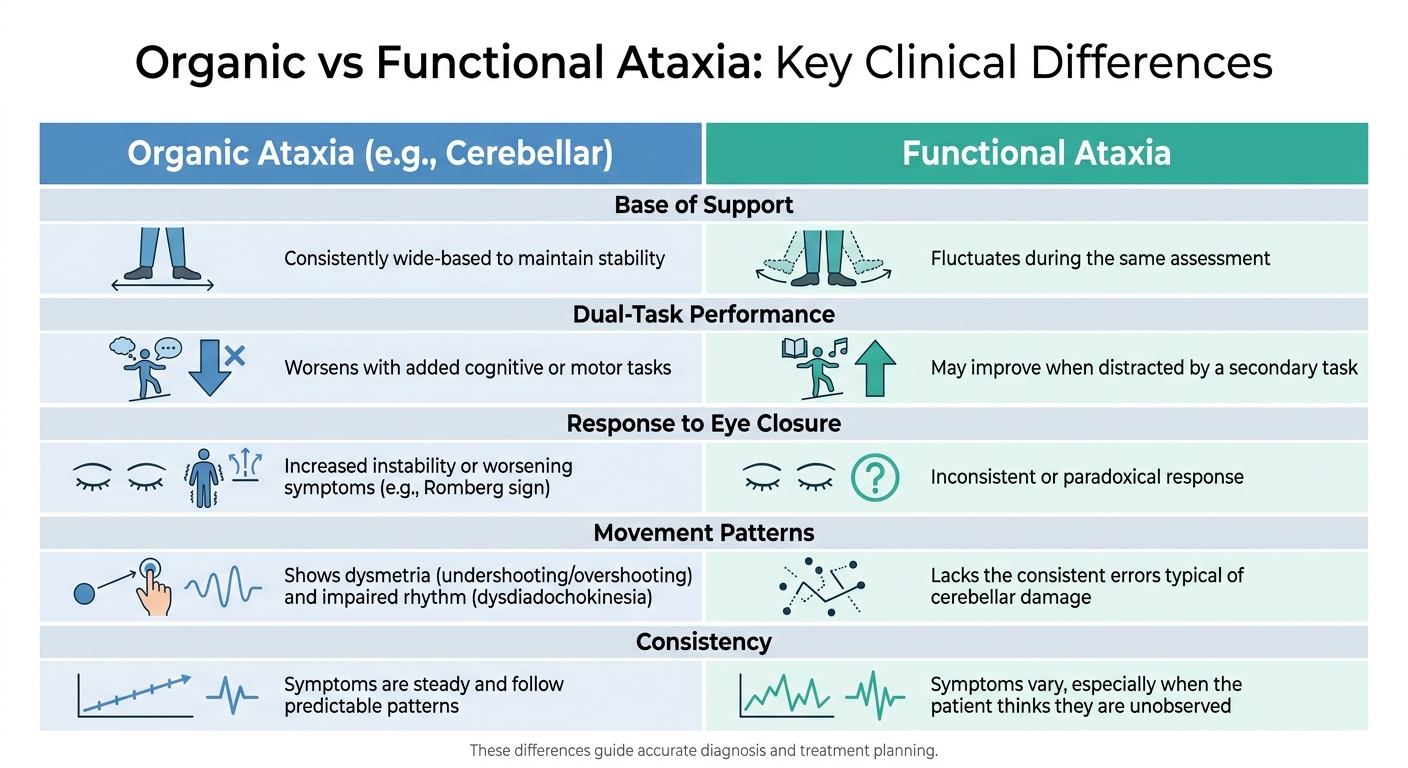
Organic vs Functional Ataxia: Key Clinical Differences
Identifying whether an ataxic gait is organic or functional is key to choosing the right assessment and treatment approach. Ataxic gait can result from a range of causes. Organic ataxic gait is linked to structural neurological damage or genetic conditions. These include disorders like Friedreich’s ataxia, spinocerebellar ataxias, Multiple System Atrophy, brain tumours, or Multiple Sclerosis. Such conditions involve the cerebellum or its pathways, disrupting how the brain processes vestibular, ocular, and proprioceptive inputs.
On the other hand, functional gait disorder is not caused by neurodegeneration. Instead, it often reflects issues with functional connectivity in the brain. This distinction is crucial because functional ataxia requires a different therapeutic approach compared to organic conditions.
Differentiating between these types of ataxia matters because many organic forms are progressive and need ongoing monitoring using tools like SARA or ICARS. Functional movement assessments, meanwhile, help pinpoint the true source of the problem, reducing the risk of misdiagnosis and ensuring treatment plans address the right concerns.
Comparison Table: Organic vs Functional Ataxia
| Feature | Organic Ataxia (e.g., Cerebellar) | Functional Ataxia |
|---|---|---|
| Base of Support | Consistently wide-based to maintain stability | Fluctuates during the same assessment |
| Dual-Task Performance | Worsens with added cognitive or motor tasks | May improve when distracted by a secondary task |
| Response to Eye Closure | Increased instability or worsening symptoms (e.g., Romberg sign) | Inconsistent or paradoxical response |
| Movement Patterns | Shows dysmetria (undershooting/overshooting) and impaired rhythm (dysdiadochokinesia) | Lacks the consistent errors typical of cerebellar damage |
| Consistency | Symptoms are steady and follow predictable patterns | Symptoms vary, especially when the patient thinks they are unobserved |
These differences highlight the importance of accurate functional assessments in shaping treatment strategies. By recognising these distinct gait patterns, clinicians can better tailor their care plans to address the specific needs of the patient.
Using Functional Assessments to Guide Care
How Chiropractors Use Functional Assessment
Functional assessments provide chiropractors with measurable insights into a patient’s coordination, balance, and posture, shaping the care they deliver. While conditions like ataxic gait often stem from neurological issues beyond chiropractic care, chiropractors can still play a role in improving posture, spinal alignment, and nervous system function as part of a multidisciplinary team.
By observing balance during standing and walking, chiropractors can identify potential stability or mobility challenges. For instance, if a patient struggles with shifting their weight or maintaining upright posture, spinal adjustments or postural retraining may help improve alignment and ease compensatory strain. This approach fits within a broader strategy aimed at supporting the nervous system and enhancing overall movement patterns.
Collaboration is key. Chiropractors often work alongside neurologists, physiotherapists, and other healthcare professionals to ensure musculoskeletal care complements wider medical or rehabilitation plans. These assessments also inform decisions about specific exercises or mobility strategies that can improve daily functioning, offering a more tailored approach to care.
Exercises and Mobility Training
Functional assessments lay the groundwork for targeted exercises aimed at addressing specific deficits. Standardised scales help pinpoint areas needing attention, such as standing balance, limb coordination, or walking speed, allowing for precise training strategies.
For patients with poor postural stability, exercises focusing on core strength and balance can be introduced. These might include supported standing drills or weight-shifting exercises to improve proprioception. If coordination tests like the Heel-to-Shin or Finger-to-Nose reveal movement inaccuracies (dysmetria), tailored coordination exercises can help retrain those motor patterns.
Gait retraining is another area guided by assessment findings. For example, results from the 8-Metre Walk Test, which evaluates walking speed and stability, can inform strategies like rhythmic pacing exercises, endurance training, or even the use of mobility aids to boost safety and confidence. Similarly, the Tandem Gait Test can highlight the need for lateral stability training to address issues like narrow-base instability.
"Severity assessment and quantification of the disability is necessary for progressive treatment plans leading to recovery and disability management." – Journal of NeuroEngineering and Rehabilitation
Conclusion: Supporting Mobility Through Functional Movement Assessments
Functional movement assessments play a key role in objectively tracking ataxic gait by measuring deficits using tools like SARA, ICARS, Heel-to-Shin, and Tandem Gait tests. These tools allow for precise care planning and effective progress monitoring. Recent reviews have highlighted their reliability in assessing cerebellar disorders.
These assessments are especially useful for tracking changes over time and determining the effectiveness of interventions. The objective data they provide not only guide clinical decisions but also fit seamlessly into broader, multidisciplinary care plans.
While ataxic gait stems from neurological issues, chiropractors can contribute by enhancing musculoskeletal function through posture correction, spinal alignment, and mobility exercises. When combined with the expertise of neurologists, physiotherapists, and other healthcare professionals, these assessments help ensure that musculoskeletal care aligns with the larger goals of improving movement and rehabilitation.
"Severity assessment and quantification of the disability is necessary for progressive treatment plans leading to recovery and disability management." – Journal of NeuroEngineering and Rehabilitation
By incorporating these assessments, individuals are empowered to take an active role in managing their condition through personalised, evidence-based care that focuses on maintaining mobility and independence.
This information is general in nature and does not replace professional medical advice. Chiropractic care addresses musculoskeletal health, and outcomes can vary. Always consult a qualified healthcare professional when making decisions about your health.
FAQs
How is ataxic gait diagnosed?
Ataxic gait is usually identified through clinical evaluations that focus on cerebellar function and coordination. Tools like the Ataxia Functional Composite Scale (AFCS), the APP-Coo-Test, and various other cerebellar function tests are commonly used. These methods aim to pinpoint movement difficulties and shed light on gait irregularities. The exact diagnostic process often depends on the clinical situation and the practitioner’s preferred approach.
Can ataxic gait be improved with exercises?
Research indicates that certain exercises can aid movement and coordination in people with ataxic gait. These often involve movement and balance-focused routines, which are commonly included in management plans to enhance motor control and stability. However, the outcomes can differ significantly from person to person. Chiropractic care, while potentially helpful for improving posture and mobility as part of overall musculoskeletal health, is not specifically designed to address ataxic gait. For personalised guidance, it’s essential to consult a healthcare professional.
When should I see a neurologist for ataxia?
If you’re experiencing sudden or worsening symptoms of ataxia, such as trouble walking or noticeable neurological changes, it’s important to see a neurologist. These issues could indicate a need for specialised care, as outlined in neurological gait assessment guidelines.