Wearable sensors are transforming how we assess and improve gait and posture by providing precise, objective movement data outside of clinical settings. These compact devices – like accelerometers, gyroscopes, and pressure sensors – track key metrics such as step length, walking speed, and joint angles. Unlike traditional lab systems, they monitor movement during daily activities, offering a clearer picture of musculoskeletal health.
Key takeaways include:
- Inertial Measurement Units (IMUs): Combine accelerometers, gyroscopes, and magnetometers for detailed 3D motion tracking.
- Pressure Sensors: Measure forces on the body, often embedded in shoe insoles, to assess balance and foot mechanics.
- Real-Time Feedback: Devices provide instant cues to correct posture and gait, aiding rehabilitation and reducing fall risks.
- Rehabilitation Support: Sensors track recovery progress with metrics like gait velocity and variability, helping clinicians personalise treatment plans.
Advances in AI and miniaturisation are making these sensors smaller, more accurate, and easier to integrate into everyday items like clothing and footwear. This technology is reshaping movement analysis, making it more accessible and practical for both individuals and healthcare professionals.
How Do Wearable Health Devices Perform Gait Analysis? – Orthopedic Support Network
sbb-itb-585d67d
Types of Wearable Sensors Used for Gait and Posture
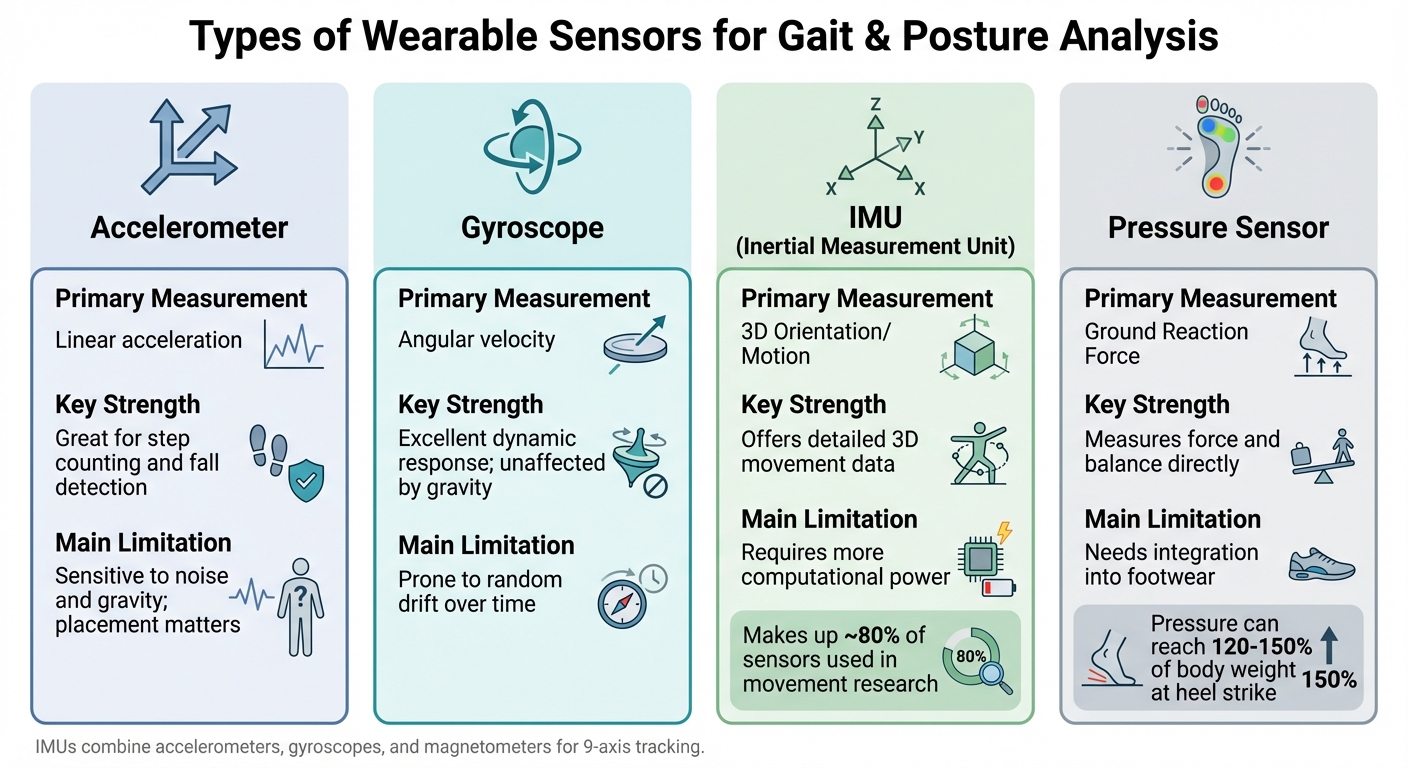
Comparison of Wearable Sensor Types for Gait and Posture Analysis
Wearable sensors come in various forms, each designed to capture specific details about how we move. By understanding how these sensors work, we can better grasp how they contribute to improving gait and posture.
Inertial Measurement Units (IMUs)
IMUs are a cornerstone of wearable gait analysis, making up roughly 80% of the sensors used in movement research. These devices combine three key components: a 3-axis accelerometer, a 3-axis gyroscope, and often a 3-axis magnetometer. Together, they provide 9-axis tracking, offering a detailed picture of body movement.
The magnetometer is particularly useful as it detects the Earth’s magnetic field, providing a reference point to correct the gyroscope’s "drift" errors over time. This ensures accurate orientation data during extended monitoring. For instance, in August 2025, a study using the GYENNO Motor Function and Motor Symptom Quantitative Assessment System evaluated 225 Parkinson’s disease participants. This system used 10 IMU sensors placed across the body – on the wrists, chest, waist, thighs, shanks, and feet – capturing data at 100 Hz. The study achieved over 80% accuracy in predicting gait and posture scores.
Accelerometers and Gyroscopes
While IMUs combine multiple sensors, accelerometers and gyroscopes can also function independently and serve specific purposes.
Accelerometers measure linear acceleration along a sensitive axis using a proof mass and mechanical suspension system. This makes them ideal for detecting step counts, gait speed, and sudden movements like falls. However, they are sensitive to noise, gravity, and their placement on the body.
Gyroscopes, on the other hand, measure angular velocity by leveraging the Coriolis effect to track rotation. They excel at capturing limb orientation during movement and are unaffected by gravity or positional shifts on rigid bodies. The downside? They tend to experience random drift over longer durations, which is why they’re often paired with accelerometers in IMUs.
Pressure and Force Sensors
Unlike inertial sensors that focus on motion, pressure and force sensors measure the forces your body exerts during movement. These sensors, often embedded in shoe insoles, use piezoelectric, strain gauge, or capacitive transducers to convert mechanical force into electrical signals.
For example, during walking, the pressure on your foot can reach 120%–150% of your body weight at heel strike and toe push-off. High-resolution systems can include sensor matrices with up to four sensors per square centimetre, enabling detailed measurements across specific foot areas like the heel, metatarsals, and toes. Between 2023 and 2024, the No Barriers Foundation Ireland used IEE Smart Foot sensors (ActiSense Kit) in a 12-week rehabilitation program. These insoles, equipped with eight high-dynamic pressure cells, tracked Centre of Pressure trajectories and stride time disparities in participants with conditions like Multiple Sclerosis, Spinal Cord Injury, and Traumatic Brain Injury. The data revealed gait abnormalities, helping clinicians create tailored rehabilitation plans. Companies like TEC GIHAN Co. in Kyoto, Japan, have even developed systems like the "M3D" sensor, which integrates 3D motion sensors and Ground Reaction Force sensors into shoes for clinical gait analysis.
By combining these diverse sensors, researchers and clinicians can achieve a more accurate understanding of movement patterns, paving the way for personalised gait and posture interventions.
| Sensor Type | Primary Measurement | Key Strength | Main Limitation |
|---|---|---|---|
| Accelerometer | Linear acceleration | Great for step counting and fall detection | Sensitive to noise and gravity; placement matters |
| Gyroscope | Angular velocity | Excellent dynamic response; unaffected by gravity | Prone to random drift over time |
| IMU | 3D Orientation/Motion | Offers detailed 3D movement data | Requires more computational power |
| Pressure Sensor | Ground Reaction Force | Measures force and balance directly | Needs integration into footwear |
How Wearable Sensors Support Gait and Posture Improvement
Wearable sensors do more than just track your movements – they actively help improve them. By combining real-time feedback with data-driven rehabilitation strategies, these devices are reshaping how we approach posture and gait correction, offering valuable insights into musculoskeletal health, often managed by a chiropractor in Sydney.
Real-Time Feedback for Posture Correction
One of the standout benefits of wearable sensors is their ability to deliver instant feedback as you go about your daily activities. Through a biofeedback loop, these systems measure your movements, classify the data, and provide immediate cues to guide corrective actions.
A fascinating example comes from a study led by Toh Yen Pang at RMIT University in October 2025. Using an IMU-based wearable system embedded with a WitMotion WT901BLECL sensor, researchers provided real-time auditory feedback to participants walking on a treadmill. The system used distinct sound cues: "whoosh" tones to signal deviations from ideal posture and "bass" tones for excessive trunk rotation. These auditory signals helped participants become more aware of specific gait phases, such as heel strikes, and adjust accordingly.
"Auditory biofeedback operates in parallel with movement, facilitating proprioceptive awareness and continuous monitoring during activity." – Toh Yen Pang et al., RMIT University
What makes these systems particularly effective is their personalisation. Each user’s ideal movement range is established, and feedback is triggered only when deviations exceed a set threshold – usually around ±5% from the baseline. This tailored approach ensures that the feedback is meaningful and relevant, paving the way for more precise rehabilitation strategies.
Using Sensor Data for Rehabilitation Plans
Beyond immediate corrections, wearable sensors play a crucial role in long-term rehabilitation. They provide objective metrics – like gait velocity, step time, and asymmetry – that complement patient-reported symptoms, giving healthcare professionals a clearer picture of recovery progress and musculoskeletal health.
A study conducted by the Wearables and Gait Analysis Research Group (WAGAR) at the Prince of Wales Private Hospital from March to June 2021 highlights this potential. Researchers tracked 12 lumbar spine surgery patients using a MetaMotionC single-point sensor attached to the sternum. They found that gait asymmetry improved by 17.4% to 60.3%, while gait variability improved by 21.0% to 65.8% after surgery. These improvements closely correlated (r = 0.581–0.914) with better scores on the Oswestry Disability Index, offering concrete evidence of surgical success during follow-up visits.
"Gait analysis using a single-point wearable sensor can demonstrate objective evidence of recovery in lumbar spine patients after surgery. This may be used as a routine pre- and postoperative assessment during scheduled visits to the clinic." – R. Dineth Fonseka, University of New South Wales
Wearable sensors also allow for continuous monitoring, revealing subtle changes in gait or posture that might go unnoticed during routine clinic visits. This remote data tracking enables healthcare providers to adjust treatment plans as needed, without requiring extra in-person appointments, making rehabilitation more personalised and responsive.
| Gait Metric Category | Role in Rehabilitation | Example Parameters |
|---|---|---|
| Spatiotemporal | Tracks overall mobility and efficiency | Gait velocity, step length, cadence |
| Asymmetry | Highlights side-to-side imbalances | Step length asymmetry, swing time discrepancy |
| Variability | Evaluates stability and fall risk | Coefficient of variation of step time |
| Kinematic | Monitors joint-specific recovery | Knee range of motion, hip flexion angles |
Using Wearable Sensors with Chiropractic and Musculoskeletal Care
Wearable sensors are starting to play a supportive role in chiropractic and musculoskeletal care by providing objective movement data. These devices go beyond patient-reported symptoms and in-clinic observations, offering measurable insights into how patients move and maintain posture in their daily lives. This data-driven approach allows practitioners to craft more tailored care plans and conduct more precise posture evaluations.
Posture Data for Chiropractic Assessments
One of the ongoing challenges in musculoskeletal care is detecting postural imbalances that can lead to discomfort or limited movement. Wearable sensors help address this by measuring deviations from "neutral posture." This term refers to a position where the head and upper trunk are aligned at zero degrees relative to the spine. Misalignment here can increase stress on intervertebral discs and potentially compress nerves.
Clinical studies have shown that sensor-derived metrics, like gait data, often align closely with patient-reported outcomes. These measurements allow practitioners to link spinal adjustments or rehabilitation exercises to tangible improvements in movement. For example, wearable sensors can track joint range of motion, step length asymmetry, and centre of pressure migration. Sensors placed near the lower back, specifically around the L3–L5 vertebrae, are particularly effective in capturing a broad range of gait and posture insights. This information helps identify areas that may benefit from targeted treatments.
Tracking Movement Patterns Over Time
Wearable sensors also shine in their ability to monitor movement patterns over extended periods, capturing data during everyday activities that would be hard to replicate in a clinical setting. This helps avoid the Hawthorne effect, where patients might unconsciously adjust their behaviour when under observation.
In chiropractic care, practitioners can use this continuous data to track changes in gait velocity, cadence, or step time variability over time. For instance, improvements such as reduced asymmetry or enhanced walking stability can provide objective evidence of treatment effectiveness. Remote monitoring capabilities further enable clinicians to assess rehabilitation progress between visits, ensuring that alignment improvements are sustained during daily routines.
Although still relatively new in clinical practice, wearable sensors offer an additional layer of insight into how bodies move and adjust over time. By combining ongoing monitoring with periodic in-clinic assessments, practitioners can refine treatment plans to achieve better results.
Future Developments in Wearable Sensor Technology
Wearable sensors are evolving to become smaller, smarter, and more integrated into everyday life. Advances in Micro-Electro-Mechanical Systems (MEMS) and Integrated Circuits (ICs) are at the heart of this transformation. For example, modern triaxial accelerometers now measure only 3–6 mm wide and 1.5 mm thick. This miniaturisation allows them to be seamlessly embedded into items like eyeglasses, smart jackets, and even socks, without interfering with natural movement or causing discomfort.
Smaller sensors also mean better accuracy. Lightweight designs reduce measurement errors caused by soft tissue artefacts – when a sensor shifts relative to the skin or muscle. By positioning these sensors closer to bony landmarks, practitioners can achieve more precise readings of joint angles, minimising noise from muscle movement. A standout development came in November 2023, when AdvanPro (based in Hong Kong) began mass production of "Softcepter" fabric sensors. These flexible sensors replace rigid components in systems monitoring muscle strength and plantar pressure, offering greater comfort and adaptability for wearers.
Beyond hardware improvements, data processing advancements are enhancing what these sensors can do. Artificial intelligence (AI) is revolutionising how sensor data is used. Machine learning algorithms now detect gait events like heel strikes and toe-offs with near-perfect accuracy during non-rotational walking phases. Deep learning takes this further, identifying abnormal gait patterns, such as Freezing of Gait, with impressive precision. AI also enables personalised solutions, as subject-dependent models learn an individual’s unique movement patterns over time, opening doors to tailored biofeedback and exercise programs.
"The latest research is moving towards Machine Learning (ML) because of high accuracy in processing the gait parameters based on application requirements." – IEEE Access
Cost and accessibility are improving too. The shift from expensive, lab-based optical motion capture systems to portable Inertial Measurement Units (IMUs) is making gait analysis more practical for everyday use. Embedded sensors in smartphones and smartwatches now enable posture monitoring without the need for specialised equipment. For instance, the Mobilise-D Consortium in Europe has developed extensive databases of gait signals to support routine, affordable clinical applications. Similarly, the University of Verona’s GPSJack (Gait and Posture Smart Jacket) project is creating low-cost prototypes using wireless 3D inertial units and machine learning to provide effective biofeedback for rehabilitation.
As wearable sensor technology continues to advance, it’s becoming more integrated into daily life. The growing accessibility of these innovations allows more people to monitor and improve their movement patterns outside of clinical environments. With research in human motion wearables producing over 1,300 papers annually by 2020, this field is rapidly advancing towards more refined, affordable, and user-friendly solutions. These developments hold the potential to revolutionise gait and posture assessments, making musculoskeletal care more accessible for everyone.
Key Takeaways
Wearable sensors are changing the way we evaluate and improve movement. By shifting from subjective observations to objective, data-driven measurements, these devices capture metrics like step length, gait velocity, and weight distribution in everyday settings. This approach enables more precise tracking of posture and gait patterns over time, especially outside of clinical environments.
One standout feature of these sensors is real-time biofeedback. By delivering immediate auditory or visual cues, these systems help users adjust their posture or movement as they go. Research highlights high user satisfaction with such systems, showing their effectiveness in promoting self-correction and motor learning without the need for constant clinical supervision.
In musculoskeletal care, wearable sensors complement traditional assessments by identifying subtle movement changes that could signal early issues, such as an increased risk of falls in older adults. They also allow practitioners to monitor patients between visits, offering a clearer view of recovery progress and enabling more tailored rehabilitation plans.
This technology is becoming more accessible and practical. Modern sensors are lightweight (some as small as 5 grams), portable, and far more affordable than lab-based motion capture systems. This makes it possible to monitor gait and posture in real-world settings – whether at home, the gym, or the workplace. By providing continuous, accurate data, these devices support ongoing movement assessment, benefiting both self-management and clinical care. For example, Dr. Ralph Jasper Mobbs and his team at Prince of Wales Private Hospital in Sydney have shown how single-point sensors can reliably track recovery during routine follow-ups, making them a practical addition to clinical practice.
"Gait analysis using a single-point wearable sensor can demonstrate objective evidence of recovery in lumbar spine patients after surgery. This may be used as a routine pre- and postoperative assessment during scheduled visits to the clinic." – R Dineth Fonseka et al., Wearables and Gait Analysis Research Group
With their ability to deliver real-time insights and support long-term care, wearable sensors are becoming essential tools for movement analysis and musculoskeletal health.
FAQs
Where should wearable sensors be placed for accurate gait data?
Wearable sensors work best when positioned on the lower back, pelvis, or limbs to gather accurate gait data. Among these, the lower back stands out as especially effective, as it provides insights into both gait patterns and posture.
How accurate are wearable sensors outside the clinic?
Wearable sensors used outside clinical settings are proving to be a dependable way to measure gait and posture. There’s some evidence suggesting these devices could play a role in clinical evaluations and help detect gait patterns in real-world environments.
Can a smartwatch or phone reliably track posture and gait?
Smartwatches and phones have the capability to monitor posture and gait, offering a glimpse into movement patterns. While research suggests they can aid in movement analysis, their accuracy and reliability are still under scrutiny. These devices can deliver general observations, but they don’t quite measure up to the precision offered by specialised equipment.





