Movement screening is a method used in chiropractic care to assess how your body moves and identify issues like limited mobility or imbalances. Instead of focusing only on areas of pain, this approach evaluates overall movement patterns to find the root cause of discomfort. Tools like the Functional Movement Screen (FMS) and Selective Functional Movement Assessment (SFMA) help chiropractors create tailored care plans, combining adjustments, exercises, and lifestyle advice. This method not only addresses pain but also improves how your body moves, reducing the risk of future injuries and supporting long-term health.
Key takeaways:
- Movement screening evaluates how your body moves as a whole.
- Tools like FMS and SFMA pinpoint dysfunctions and guide treatment.
- Care plans include chiropractic adjustments, corrective exercises, and posture/lifestyle advice.
- Regular follow-ups track progress and adjust plans as needed.
This approach ensures treatments target the underlying causes of pain, helping you move better and feel stronger.
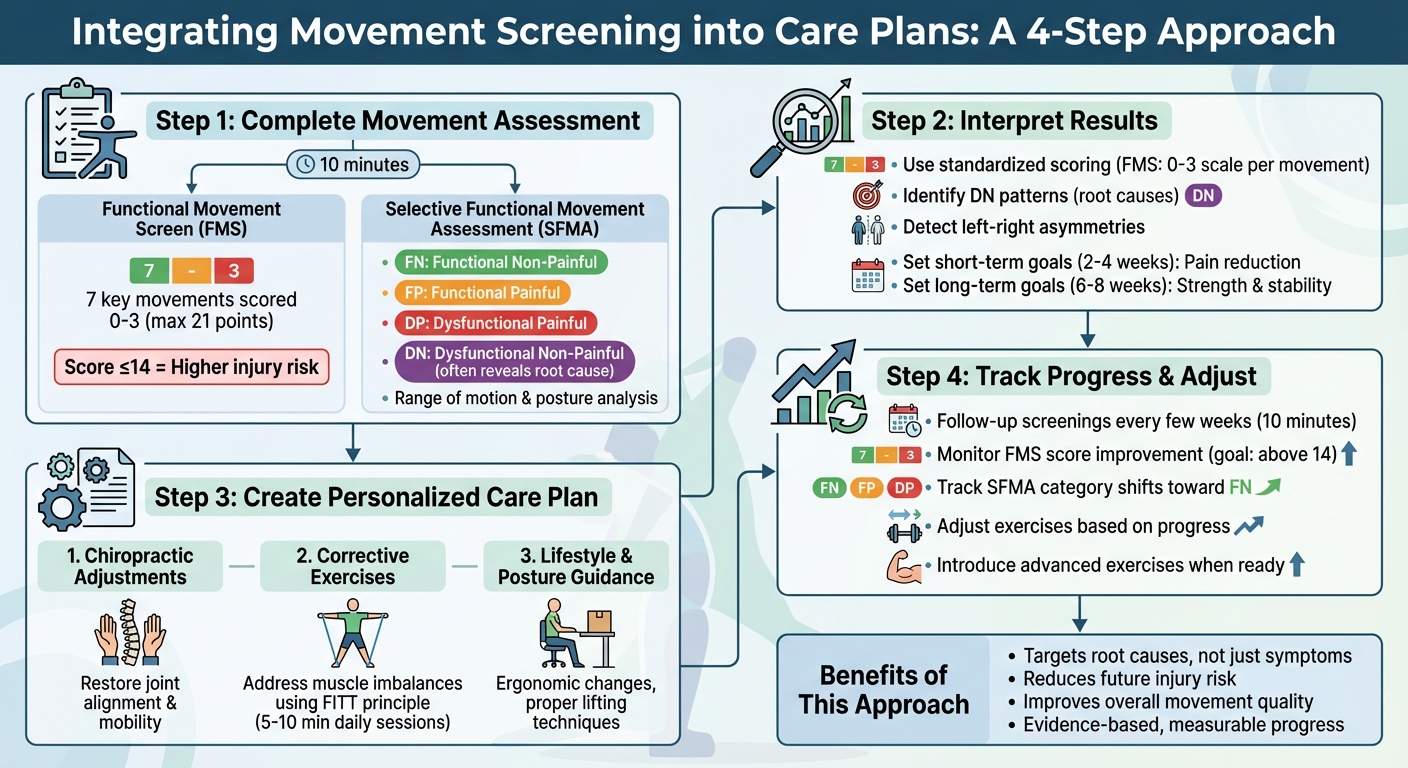
4-Step Movement Screening Integration Process for Chiropractic Care
Functional Movement Screen │ Evaluation for FSP Patient
sbb-itb-585d67d
Step 1: Performing a Complete Movement Assessment
Before creating a personalised care plan, it’s essential to establish a baseline of how the body moves as a whole. This initial assessment, which takes about 10 minutes, provides crucial data to guide treatment. It focuses on how different parts of the body work together during everyday movements.
Functional Movement Evaluation
The process starts with observing basic movement patterns. A tool often used is the Functional Movement Screen (FMS), which evaluates seven key movements: deep overhead squat, hurdle step, in-line lunge, shoulder mobility, active straight-leg raise, trunk stability push-up, and rotary stability. A score of 14 or lower (out of 21) indicates a higher risk of injury and highlights areas that need attention.
For individuals already experiencing musculoskeletal pain, the Selective Functional Movement Assessment (SFMA) provides a deeper look. It categorises movement into four groups: Functional Non-Painful (FN), Functional Painful (FP), Dysfunctional Painful (DP), and Dysfunctional Non-Painful (DN). Interestingly, DN patterns often reveal the root cause of localised pain.
"It is the Dysfunctional Non-Painful (DN) pattern that will most often lead us to the source of a regional problem causing local pain." – Robert "Skip" George, DC
In addition to these movement evaluations, assessing range of motion and posture helps uncover specific dysfunctions.
Range of Motion and Posture Analysis
Beyond the movement pattern scores, practitioners assess joint mobility and posture, using both manual methods and digital tools. Apps like Posture Screen enable practitioners to record movements and analyse them frame by frame. This helps identify subtle issues, such as knees caving inward during a squat or feet turning outward while walking. These details reveal which muscles are overactive or underactive, aiding in treatment planning.
For example, in January 2020, Dr Brian Jensen from Cave Spring Chiropractic used the Posture Screen app to evaluate a patient with sciatic pain. The initial squat test showed the patient’s knee and feet turning outward. After testing with proprioceptive orthotics, the app revealed no movement distortions, confirming that the feet were the main source of the problem. This allowed for a focused care plan without unnecessary corrective exercises.
Step 2: Interpreting Screening Results for Personalised Care
After completing a movement assessment, the next step is to make sense of the results. This process helps chiropractors design specific treatment plans instead of relying on a generic approach. By analysing the screening data, practitioners can focus on the root causes of dysfunction and set clear, realistic treatment goals tailored to the individual.
Pinpointing Dysfunction and Imbalances
Standardised scoring systems are key to identifying movement issues during screenings. For example, the Functional Movement Screen (FMS) uses a scale from 0 to 3 for each movement pattern. A score of 0 indicates pain or the inability to perform the movement, while a 3 represents ideal movement. A score of 2 suggests the movement was completed but with compensation, such as favouring one side.
The Selective Functional Movement Assessment (SFMA) takes this further by focusing on Dysfunctional Non-Painful (DN) patterns. These patterns often point to deeper issues that may be contributing to pain elsewhere. For instance, someone experiencing shoulder pain might show a DN pattern in their upper back. Addressing this dysfunction could alleviate the shoulder pain – a concept known as regional interdependence.
Tests like the Hurdle Step and Inline Lunge can reveal left-right asymmetries in movement. These imbalances might indicate that one hip has limited mobility while the other compensates, or that one leg has weaker stabilising muscles. Understanding whether the issue stems from restricted mobility or stability weakness helps guide the treatment approach, whether it’s adjustments, stretching, or strengthening exercises.
Once dysfunctions are identified, the focus shifts to setting specific goals for improvement.
Establishing Goals for Progress
Using the screening data, chiropractors can set achievable, step-by-step objectives. If a movement scores a 0 due to pain, the first priority is to manage the pain before moving on to corrective exercises. Short-term goals, typically over 2–4 weeks, aim to reduce pain and restore basic function. Longer-term goals, spanning 6–8 weeks, are aligned with the body’s natural healing process and focus on building strength, stability, and resilience.
These goals are tailored to the individual’s fitness level, daily activities, and movement demands. By basing care plans on measurable data, practitioners create a structured path to help patients move better and feel stronger.
Step 3: Creating and Applying a Personalised Care Plan
After interpreting movement screening results, the next step is to create a care plan tailored to the specific dysfunctions identified. This plan combines chiropractic adjustments, corrective exercises, and lifestyle tweaks, each addressing different aspects of movement and discomfort. Together, they form a structured pathway from assessment to improvement, aiming to enhance movement quality and reduce discomfort.
Adding Chiropractic Adjustments
Chiropractic adjustments focus on restoring proper joint alignment and mobility. For example, if screening reveals limited thoracic rotation, adjustments can help improve the range of motion and potentially ease discomfort. These adjustments are particularly valuable when structural misalignments disrupt functional movement. Take the Deep Squat test: if a patient struggles due to limited ankle or hip mobility, addressing joint restrictions in these areas can support better movement patterns.
However, adjustments work best when combined with targeted exercises. While adjustments restore joint function, exercises reinforce proper muscle activation and balance.
"The adjustment makes sure that all the bones are functioning properly where the exercises are supporting proper muscular function. That’s why they go hand in hand." – Dr. Kyle Smerglia, Chiropractor
Including Corrective Exercises
Corrective exercises are designed to address specific muscle imbalances and movement issues uncovered during screening. For instance, if the Functional Squat test shows the knees collapsing inward, it often points to overactive muscles like the piriformis and tensor fasciae latae (TFL) and underactive muscles such as the gluteus maximus and adductors. A tailored exercise plan would include stretches for the tight muscles and strengthening exercises for the weak ones.
These exercises not only complement adjustments but also build functional strength and improve coordination. Following the FITT principle – Frequency, Intensity, Time, and Type – patients may begin with short, daily sessions of 5–10 minutes to establish muscle memory. As movement patterns improve, the frequency may decrease. Common exercises include core stability drills, hip mobility routines, and progressive strength training, all tailored to the seven fundamental movement patterns assessed during screening. Lifestyle advice is also provided to ensure progress is maintained.
Lifestyle and Posture Guidance
Even the best adjustments and exercises can be undermined by poor daily habits. Lifestyle guidance focuses on modifying behaviours and environments to support long-term improvement. This could include ergonomic changes, like raising a computer monitor to reduce neck strain, or teaching proper lifting techniques to protect the lower back.
Posture advice is particularly important for those with sedentary jobs or repetitive tasks. Small adjustments – such as taking regular breaks to stretch or ensuring your chair height supports a neutral spine – can go a long way in preserving the benefits of treatment. Some practitioners also use proprioceptive testing to assess whether custom orthotics might enhance movement. For example, if wearing test orthotics during a functional squat improves performance, they might be added to the care plan to create a more balanced foundation for the body’s entire kinetic chain.
Step 4: Tracking Progress and Adjusting Care Plans
After creating a personalised care plan, keeping track of progress is essential. Movement patterns change as the body responds to treatment, so a care plan should never remain static. Regular follow-ups ensure the treatment stays effective, identifying whether the exercises and adjustments are working or if changes are needed. Without these reassessments, it’s easy to overlook compensatory patterns or push the body beyond its limits too soon. Using standardised tools for these updates ensures that progress is measurable and meaningful.
Measuring Progress with Follow-Up Screenings
Follow-up screenings rely on the same methods used during the initial assessment, making it easier to track changes over time. For example, the Functional Movement Screen (FMS) evaluates seven movement patterns, assigning scores from 0 to 3 for each, with a maximum score of 21. A score of 14 or below signals a higher risk of injury, so moving above this threshold becomes a critical goal. These screenings are quick – typically taking about 10 minutes – and can be scheduled every few weeks to monitor improvement.
For patients experiencing pain, the Selective Functional Movement Assessment (SFMA) offers valuable insights. It categorises movements into four groups: Functional Non-Painful (FN), Functional Painful (FP), Dysfunctional Painful (DP), and Dysfunctional Non-Painful (DN). The aim is to shift movements into the functional and more comfortable category. These results help guide the next steps in treatment, ensuring the care plan evolves alongside the patient’s progress.
Updating Plans for Long-Term Results
Once progress is tracked, care plans can be fine-tuned to match the patient’s current abilities. For instance, an improvement in FMS score from 12 to 16 might suggest it’s time to introduce more advanced exercises or reduce the frequency of corrective drills. On the other hand, if pain returns or progress stalls, it may be necessary to revisit other problem areas in the kinetic chain.
This approach ensures that fitness gains align with improved movement quality. As patients progress, the focus can shift from corrective exercises to building strength and enhancing performance. Regular reviews not only guide these adjustments but also provide patients with a clear view of their progress. Seeing tangible results can motivate them to stick with the care plan, even after acute pain subsides. This ongoing process helps prevent future injuries and supports long-term musculoskeletal health.
Conclusion: The Benefits of Movement Screening in Chiropractic Care
Movement screening has the potential to transform chiropractic care by shifting the focus from simply addressing pain to uncovering the underlying movement patterns contributing to musculoskeletal discomfort. By identifying imbalances or asymmetries – even in areas that don’t feel painful – practitioners gain a deeper understanding of the root causes of issues rather than just treating the symptoms. For instance, a stiff hip might be a hidden factor behind lower back pain, even if the hip itself feels fine.
Tools like the Functional Movement Screen (FMS) and Selective Functional Movement Assessment (SFMA) provide measurable benchmarks that can guide treatment strategies. Research even links an FMS score below 14 to a higher risk of injury, making these tools valuable for proactive care.
Incorporating movement screening into chiropractic care can also support long-term health strategies. Instead of waiting for pain to resurface, patients can focus on improving movement quality, strength, and coordination. This proactive approach not only helps preserve essential movement skills for healthy ageing but may also lower the chances of future injuries. It highlights the importance of a dynamic and forward-thinking approach to care.
By combining chiropractic adjustments with corrective exercises and lifestyle recommendations, movement screening enables practitioners to create tailored, evidence-based care plans. This ensures that strength and function are built on a foundation of efficient and effective movement patterns, supporting patients in maintaining an active and healthier lifestyle.
This information is general in nature and is not a substitute for professional medical advice.
Chiropractic care focuses on musculoskeletal health and results vary between individuals.
Please consult a qualified healthcare professional before making decisions about your health.
FAQs
Do I need movement screening if I’m not in pain?
Movement screening is a way to evaluate how your body moves, even if you’re not currently dealing with pain. By doing this, it can pinpoint areas of weakness, imbalances, or restrictions that might set you up for injuries or movement problems down the road. Taking this kind of proactive step can help you keep your body moving well and minimise potential problems in the long run.
What’s the difference between FMS and SFMA?
The Functional Movement System (FMS) and the Selective Functional Movement Assessment (SFMA) serve distinct purposes, tailored to different situations.
FMS is designed as a screening tool to evaluate movement patterns, detect imbalances, and highlight potential injury risks in individuals who are not currently experiencing pain. Its primary goal is prevention – spotting issues before they lead to injuries.
In contrast, SFMA is intended for individuals dealing with pain. It focuses on identifying specific movement dysfunctions that might be causing or contributing to their symptoms. Essentially, while FMS is about prevention, SFMA takes a diagnostic approach to address existing problems.
How often should I be re-screened?
Reassessing movement patterns and symptoms should happen at intervals that make sense for each person’s situation and progress. Typically, it’s a good idea to schedule a re-screening when noticeable changes occur, whether in movement, symptoms, or overall condition. For regular monitoring, many opt to do this every few months. This approach ensures any improvements are tracked and care plans can be adjusted accordingly.