Functional Movement Screening (FMS) is a tool chiropractors use to assess how well your body performs basic movements. It identifies movement issues that could lead to pain or injury, focusing on seven specific patterns like squatting, lunging, and shoulder mobility. Each movement is scored from 0 to 3, with scores below 14 suggesting a higher injury risk. Chiropractors use these results to create tailored care plans, combining corrective exercises and manual therapies to improve mobility and stability.
Key Points:
- What FMS Does: Evaluates movement patterns to detect weaknesses or restrictions.
- Why It Matters: Scores below 14 triple the likelihood of injury.
- How It’s Used: Guides chiropractors in designing personalised treatments, including exercises and adjustments.
- Time Required: The screening takes about 10 minutes.
FMS works alongside other assessments like posture and gait analysis to provide a full picture of your movement health. By addressing movement issues early, it helps prevent injuries and supports long-term musculoskeletal health.
Movement Screening, Testing, and Assessment, with Gray Cook | NSCA.com
sbb-itb-585d67d
The 7 Movement Patterns in FMS
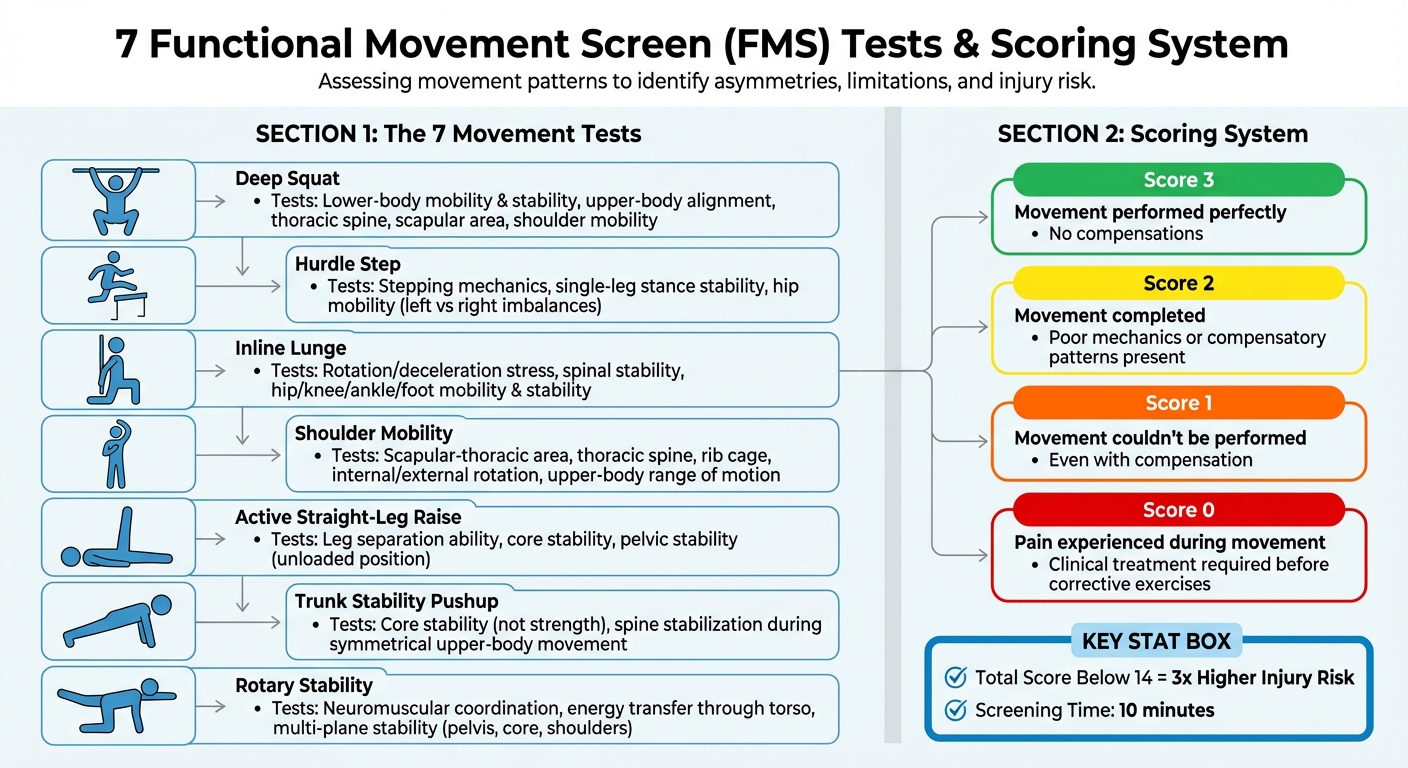
7 Functional Movement Screen Tests and Scoring System
The seven tests in the Functional Movement Screen (FMS) are designed to evaluate your mobility, stability, and coordination. Together, they give chiropractors a comprehensive view of how well your body moves as a whole. Each test reveals specific insights into your musculoskeletal system, making this more than just a fitness assessment – it’s a way to understand how your body functions.
Breaking Down Each Movement Test
Each FMS test focuses on a distinct movement pattern, offering detailed feedback about your body’s mechanics.
The Deep Squat evaluates lower-body mobility and stability while also testing upper-body alignment. Holding a dowel overhead during the movement challenges your thoracic spine, scapular area, and shoulder mobility.
The Hurdle Step looks at stepping mechanics and single-leg stance stability. It also examines hip mobility on both sides, helping to identify any imbalances between your left and right sides that could lead to compensatory movements during walking or running.
The Inline Lunge replicates the stresses experienced during rotation, deceleration, and lateral movements. Performed in a split stance on a narrow base, this test assesses spinal stability along with the mobility and stability of your hips, knees, ankles, and feet.
Shoulder Mobility focuses on the scapular-thoracic area, the thoracic spine, and the rib cage. This test combines internal rotation and adduction on one side with external rotation and abduction on the other, assessing your upper-body range of motion.
The Active Straight-Leg Raise measures your ability to separate your legs while maintaining stability in your core and pelvis, all in an unloaded position.
The Trunk Stability Pushup evaluates core stability rather than upper-body strength. It tests your ability to stabilise your spine during a symmetrical upper-body movement, requiring core engagement before arm movement.
Rotary Stability is the most complex of the tests. It assesses neuromuscular coordination and the transfer of energy through your torso. This test examines multi-plane stability in your pelvis, core, and shoulders during movements that involve both the upper and lower body.
Scoring the FMS Results
Each test is scored to pinpoint areas that may need improvement. A score of 3 means the movement was performed perfectly without any compensations. A 2 indicates the movement was completed but with poor mechanics or compensatory patterns. A 1 means the movement couldn’t be performed even with compensation, and a 0 is recorded if pain is experienced at any point during the movement.
If a score of 0 is given due to pain, clinical treatment is necessary before starting corrective exercises. Tests like the Hurdle Step and Inline Lunge can also highlight asymmetries between the left and right sides, offering valuable clues about imbalances that might need targeted intervention. These scores guide chiropractors in creating tailored care plans to address specific dysfunctions, ensuring corrective strategies are precise and effective. Each score plays a vital role in shaping ongoing assessments and interventions.
Using FMS with Other Assessment Methods
The Functional Movement Screen (FMS) works hand-in-hand with other evaluation techniques to offer a well-rounded view of body movement and uncover potential dysfunctions. Chiropractors often pair FMS findings with other methods to pinpoint not just where discomfort occurs, but also the movement patterns contributing to it.
FMS Alongside Posture and Gait Assessment
Static posture assessments focus on alignment while the body is at rest. FMS, on the other hand, evaluates how well this alignment holds up during daily movements. For instance, the In-Line Lunge assesses whether proper alignment is maintained during dynamic motion. Similarly, the Hurdle Step challenges stepping mechanics and single-leg stability, providing insights that complement traditional gait analysis. Combining these static and dynamic assessments helps identify regional interdependence – where an issue in one area, like limited hip mobility, might lead to discomfort elsewhere, such as the lower back. By uncovering these "weak links" in the kinetic chain that static assessments might miss, FMS enables more precise corrective strategies. This approach bridges the gap between static evaluations and real-world movement analysis.
FMS for Pain Management and Injury Prevention
FMS is particularly valuable for identifying movement dysfunctions in people who may not yet show symptoms. By spotting these imbalances early, practitioners can intervene before they develop into more serious issues. If pain arises during an FMS test, chiropractors often turn to the Selective Functional Movement Assessment (SFMA), a tool designed to investigate the root causes of musculoskeletal pain. The SFMA helps distinguish between mobility problems, like restricted tissue extensibility, and stability issues related to motor control. This ensures that treatment targets the underlying cause rather than just alleviating symptoms.
Additionally, FMS identifies "Dysfunctional Non-Painful" (DN) movement patterns – movements that are flawed but not painful. These patterns highlight areas that could benefit from corrective exercises, reducing the risk of chronic problems and future injuries. Together, FMS and complementary assessments create tailored care plans that address specific movement impairments and support long-term health.
Treatment Approaches Based on FMS Findings
Treatment strategies based on the Functional Movement Screen (FMS) are carefully designed to address specific movement limitations. Chiropractors use FMS results to create a personalised care plan, often following the "3 R’s" method: Reset, Reinforce, and Retrain. This step-by-step process lays the groundwork for lasting improvements in movement and function.
When pain is present (indicated by a score of 0), it becomes the immediate priority. Clinical interventions like adjustments or soft tissue therapy are applied before starting corrective exercises. This is critical because trying to strengthen or stretch a painful area without resolving the underlying issue can reinforce poor movement patterns and potentially worsen the problem.
Corrective Exercises for Movement Problems
Corrective exercises are tailored to address the weak points identified by FMS. For example, a low score on the Active Straight-Leg Raise highlights the need for better hip mobility and core stability. Exercises like hamstring extensions, performed while keeping the opposite leg flat, can help improve hip dissociation – allowing one hip to move independently without disrupting pelvic alignment.
For individuals who struggle with the Hurdle Step, single-leg stance exercises against a door frame can help build stability. The focus here is on maintaining a level hip while stepping, ensuring proper alignment. Poor performance on rotation tests often requires quadruped thoracic rotation exercises. These involve kneeling on all fours, placing one hand behind the head, and rotating the elbow down and up to enhance spinal mobility.
The Trunk Stability Push-Up test often reveals core control issues. To address this, practitioners may recommend exercises that focus on reflex core bracing – engaging the abdominal muscles before initiating upper body movement. This helps prevent compensatory patterns like hip sagging or shifting, which occur when core stability is lacking.
How Adjustments Support Better Movement
Manual therapies play a key role in improving movement mechanics alongside corrective exercises. Spinal adjustments, for instance, can address joint restrictions that limit mobility, complementing the benefits of targeted exercises.
Movement is not just the muscles moving joints or bones, it is a complex information pathway between your nervous system and the rest of the body.
Adjustments optimise this pathway, especially when FMS highlights mobility restrictions in areas like the thoracic spine or hips. For example, someone who struggles with the Shoulder Mobility test may have limited thoracic spine movement. Chiropractic adjustments in this region can help restore mobility, allowing thoracic rotation exercises to be more effective. Without resolving joint restrictions first, exercises alone may not lead to meaningful progress.
Progress is monitored using the test-retest method. If a movement pattern doesn’t improve after a week of corrective exercises, it often indicates a deeper issue, such as a joint or tissue restriction, that requires hands-on treatment. This combination of manual therapy and targeted exercises helps establish a strong foundation of mobility and stability, reducing the likelihood of future injuries and enhancing overall function.
Summary
The Functional Movement Screen (FMS) gives chiropractors a structured way to assess overall body movement instead of zeroing in solely on the pain point. By evaluating seven key movement patterns, it helps identify imbalances, restricted mobility, or stability issues that may lead to musculoskeletal problems or increase injury risk.
As Gray Cook puts it:
"Movement is how we survive, communicate, recreate and thrive." – Gray Cook, Author of Movement: Functional Movement Systems
This assessment uses an objective scoring system to establish a baseline for movement. Research indicates that scores below 14 could significantly raise the risk of injury, highlighting its value in spotting movement inefficiencies early.
When combined with manual therapies and targeted corrective exercises, FMS results can guide treatment plans and track progress through a test-retest method. These scores provide actionable insights for tailoring care. For patients experiencing pain, the Selective Functional Movement Assessment (SFMA) offers a more detailed diagnostic approach.
A strong functional base – ensuring proper mobility and stability – can prepare individuals for a gradual return to more challenging activities. This method aims to improve movement quality, minimise compensatory patterns, and support long-term musculoskeletal health.
This information is general and not a substitute for professional medical advice. Chiropractic care focuses on musculoskeletal health, and outcomes vary by individual. Always consult a qualified healthcare professional before making decisions about your health.
FAQs
Is FMS right for me if I’m not in pain?
Functional Movement Screening (FMS) isn’t just for those dealing with pain. It’s a way to evaluate how your body moves, pinpoint any limitations or imbalances, and create tailored exercises to address them. By doing so, FMS can enhance the way you move and may lower the chances of potential problems down the track.
What happens if a test causes pain or scores 0?
If a test results in pain or scores a 0, it’s seen as a red flag. This could point to movement issues or discomfort linked to that particular action. These findings often indicate the need for a deeper evaluation to uncover and address the root cause.
How often should FMS be re-tested?
The timing for re-testing Functional Movement Screening (FMS) depends on personal goals and specific needs. A common recommendation is to re-test every few months. This approach helps monitor progress and allows for adjustments to your care plan, ensuring ongoing improvement in movement patterns.