Chronic pain affects millions in Australia, but the right diet can help manage symptoms by reducing inflammation and supporting overall health. Here’s what you need to know:
- Inflammation and Pain: Persistent inflammation worsens pain sensitivity. Avoid processed foods, refined sugars, and trans fats, which can trigger inflammation. Focus on whole foods like vegetables, fruits, and healthy fats to calm the immune system.
- Gut Health: High-fibre foods (e.g., oats, lentils) promote good gut bacteria, reducing inflammation. Limit alcohol, as it disrupts gut health and increases pain sensitivity.
- Anti-Inflammatory Diets: Diets like the Mediterranean diet, rich in olive oil, fatty fish, and legumes, can lower pro-inflammatory markers and help with conditions like arthritis and fibromyalgia.
- Key Nutrients: Omega-3s (salmon, flaxseeds), magnesium (leafy greens, seeds), and vitamin D (dairy, sardines) support nerve and muscle function, reduce fatigue, and improve mood.
- Daily Habits: Stay hydrated, maintain a healthy weight, and eat at regular intervals to stabilise blood sugar and reduce nerve sensitivity.
- Spices: Turmeric and ginger have anti-inflammatory properties and can be easily added to meals.
For best results, combine these dietary changes with physical activity, stress management, and professional care like chiropractic adjustments. Small improvements may appear in weeks, with more noticeable changes in 2–3 months. Always consult a healthcare professional before making significant dietary changes.
Dietitian Reveals Power of Anti-inflammatory Diet – Chronic Pain – The Pain Diaries Podcast
sbb-itb-585d67d
Anti-Inflammatory Diet Basics
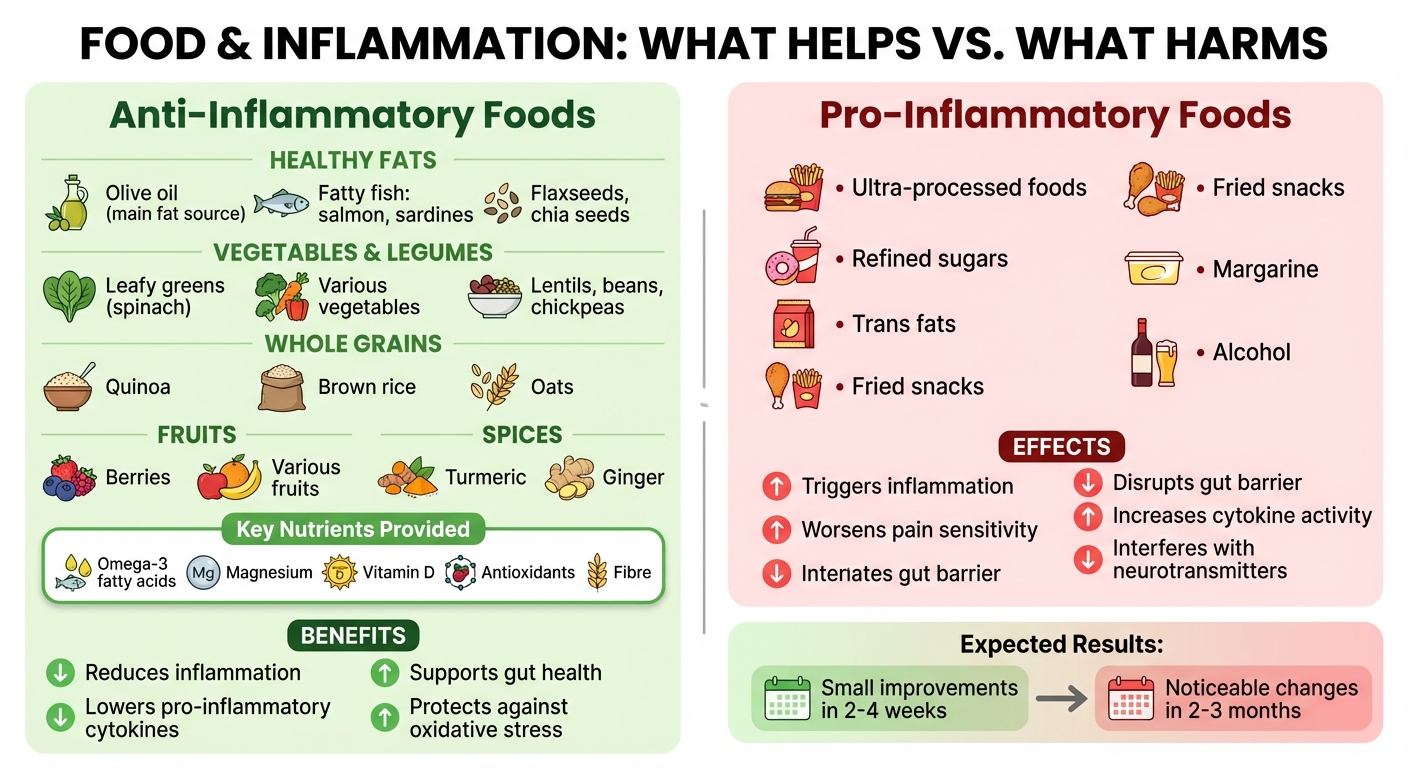
Anti-Inflammatory Foods vs Pro-Inflammatory Foods for Pain Relief
An anti-inflammatory diet centres on whole, unprocessed foods packed with fibre, antioxidants, and healthy fats. This way of eating aims to reduce low-grade chronic inflammation, which can intensify pain. Diets like the Mediterranean and DASH diets naturally align with these principles and have been studied for their health benefits.
The Mediterranean Diet for Pain Management
The Mediterranean diet is often highlighted for its potential in managing chronic pain. It features olive oil as the main fat source, alongside fatty fish like salmon and sardines, whole grains such as quinoa and brown rice, and a variety of vegetables and legumes. Research suggests that people with fibromyalgia may find pain relief and improved quality of life by following this diet. Similarly, studies on knee arthritis show that consuming pro-inflammatory foods can speed up disease progression, while a Mediterranean-style diet may help slow it down.
The effectiveness of this diet lies in its ability to lower pro-inflammatory cytokines and deliver antioxidants. Key components like olive oil, berries, and turmeric provide protection against oxidative stress, which can damage nerves over time.
Foods That May Help: Vegetables, Fruits, and Healthy Fats
Incorporating specific food groups into your diet can further aid in natural pain relief. Omega-3-rich foods, such as salmon, sardines, and flaxseeds, are known to combat inflammation at the cellular level. Magnesium-rich options, including spinach, seeds, and legumes, support nerve and muscle function. For those watching their budget, frozen vegetables, canned beans, and bulk grains like oats and lentils are cost-effective ways to enjoy these benefits.
On the flip side, ultra-processed foods, refined sugars, and trans fats – commonly found in fried snacks and margarine – can trigger inflammation and worsen pain. Alcohol is another factor to limit, as it can disrupt the gut barrier, increase cytokine activity, and interfere with neurotransmitters that help soothe the nervous system.
Nutrients That May Support Pain Relief
Certain nutrients can complement an anti-inflammatory diet by aiding the body’s natural pain management processes. Below are some key nutrients that may play a role in reducing pain and inflammation.
Omega-3 Fatty Acids and Inflammation
Omega-3 fatty acids can help reduce inflammation by decreasing the production of pro-inflammatory cytokines – molecules that signal the immune system to initiate inflammation. By doing so, omega-3s might help regulate pain responses and reduce central sensitisation, a condition where the nervous system becomes overly sensitive to pain. Additionally, they may help manage brain inflammation, potentially alleviating secondary symptoms like fatigue and mood changes often linked to chronic pain.
You can find omega-3s in fatty fish such as salmon and sardines, as well as plant-based sources like flaxseeds and chia seeds. Regular consumption over several weeks may lead to noticeable benefits. However, if you’re on blood thinners, it’s wise to consult a healthcare professional before increasing your omega-3 intake, as interactions may occur.
Magnesium and Vitamin D for Pain Management
Magnesium and vitamin D both play important roles in supporting nerve, muscle, and immune function, which are critical to managing chronic pain. Magnesium helps regulate nerve signals and muscle activity, while vitamin D supports bone health and immune cell function. Both nutrients may also influence mood and reduce fatigue, which are common issues for those dealing with chronic pain.
| Nutrient | Role in Pain Management | Food Sources |
|---|---|---|
| Magnesium | Supports nerve and muscle function; may reduce fatigue | Leafy greens, seeds, legumes |
| Vitamin D | Aids bone and immune health; may ease inflammation | Dairy (milk), salmon, sardines |
Whole foods are the best way to get these nutrients, as they provide a balanced intake without the risk of over-supplementation. Supplements should only be used to address specific deficiencies, and it’s important to consult a healthcare provider before starting them.
Turmeric and Ginger: Anti-Inflammatory Spices
Turmeric and ginger are known for their anti-inflammatory properties, which can support the body’s healing processes. Turmeric contains antioxidants that protect nerve cells from oxidative damage and help maintain immune balance. Both spices may help reduce low-grade inflammation associated with chronic pain and conditions like central sensitisation.
Incorporating these spices into meals is simple. For instance, you can add turmeric to a chickpea and sweet potato curry with brown rice, or use ginger in teas or stir-fries. Pairing turmeric with healthy fats, such as olive oil, can boost its absorption and effectiveness. However, if you’re taking blood thinners or have certain gut conditions, it’s best to consult a doctor or dietitian before increasing your intake, as turmeric might interact with some medications.
Daily Habits That Support Pain Management
Simple daily habits like staying hydrated, managing weight, and eating at consistent times can play a big role in managing chronic pain. These strategies, combined with an anti-inflammatory diet, can help support your nervous system and ease pressure on your joints.
Staying Hydrated and Managing Weight
Drinking enough water is key when it comes to pain management. Staying hydrated with water or herbal teas – like peppermint tea – can help soothe your body and may reduce central sensitisation. On the other hand, alcohol can increase inflammation and is best avoided.
Keeping your weight in a healthy range also helps reduce strain on your joints and may even slow the progression of conditions like knee arthritis. Research shows that around 32% of people seeking chronic pain treatment are overweight, while 39% are classified as obese[2]. If weight management feels overwhelming, a dietitian can create a plan tailored to your needs. Simple swaps, like replacing sugary drinks with water or unsweetened herbal teas, can help you stay hydrated without triggering pain flare-ups.
Hydration and weight control are vital, but meal timing is another often-overlooked factor in managing chronic pain.
Meal Timing and Portion Sizes
Eating at regular intervals can stabilise your blood sugar levels, which may reduce nerve sensitivity and help manage pain. Fluctuating blood sugar is linked to increased pain sensitivity, and many people with chronic pain consume more calories than they need – leading to weight gain and worsening symptoms.
To keep your energy steady and support gut health, aim for three balanced meals and a healthy snack each day. Focus on vegetables, fruits, and healthy fats, and prioritise nutrient-rich foods over calorie-dense options. Budget-friendly staples like frozen veggies, canned beans, and bulk grains (such as oats and lentils) make meal planning more accessible and help with portion control. Adding fibre-rich foods to your diet can also improve your gut microbiome, which plays a key role in reducing inflammation.
Combining Nutrition with Other Pain Management Approaches
Nutrition works best when paired with other proven pain management methods. Tackling inflammation through diet while also focusing on musculoskeletal health can create a more solid path to long-term relief. Let’s look at how chiropractic care can complement these nutritional strategies.
Chiropractic Care and Nutrition Working Together
Chiropractic care is all about improving musculoskeletal health, focusing on posture, spinal alignment, and the nervous system. When paired with an anti-inflammatory diet, this combination can provide even greater support for your body.
Certain nutrients align well with chiropractic goals. For instance, magnesium – found in foods like leafy greens, seeds, and legumes – plays a role in nerve and muscle function, aiding muscle relaxation and recovery after adjustments. Similarly, omega-3 fatty acids from salmon, sardines, and flaxseeds can help lower pro-inflammatory cytokines, which might assist in calming an overactive nervous system, especially in cases of central sensitisation.
If you’re in Bondi Junction, Dr Steve offers chiropractic care that focuses on gentle, nervous-system-based adjustments. This approach complements an anti-inflammatory diet by improving posture, spinal health, and natural pain relief. Together, these methods can ease morning stiffness and boost energy levels within a few weeks. For noticeable, lasting changes, consistency over 2–3 months is often key.
Adding Exercise and Stress Management to Your Plan
To truly tackle chronic pain, movement and stress reduction are essential additions to your plan. These elements work hand-in-hand with diet and physical care for a more rounded approach.
Low-impact exercises like walking, swimming, or yoga can enhance flexibility and ease joint stiffness, making your body more receptive to dietary and physical therapies. On the other hand, mindfulness practices, deep breathing, and quality sleep help calm the nervous system and promote healing. Cutting out alcohol is especially important – it disrupts the gut barrier, interferes with calming neurotransmitters, and reduces the quality of restorative sleep. Together, these lifestyle changes can amplify the benefits of your pain management strategy.
Getting Started with Nutritional Pain Relief
Main Points to Remember
To kick off your journey toward nutritional pain relief, keep these essentials in mind. Think of it as a lifestyle shift rather than a temporary fix. Diets like the Mediterranean and DASH provide excellent starting points, focusing on fresh, whole foods such as vegetables, fruits, healthy fats, and whole grains. Instead of obsessing over what to eliminate, concentrate on adding foods that nourish your body and support your overall health. These dietary choices align with earlier strategies aimed at reducing inflammation and promoting a healthy nervous system.
Key nutrients play a big role here. Omega-3 fatty acids from fish like salmon and sardines, magnesium from leafy greens and seeds, and anti-inflammatory spices like turmeric and ginger are excellent additions. At the same time, try cutting back on ultra-processed foods, refined sugars, trans fats, and alcohol, as these can disrupt nervous system balance. You might notice small changes, like improved gut health, better energy, or reduced morning stiffness, within 2–4 weeks. For lasting pain relief, consistency is key – stick with these changes for 2–3 months.
To take your pain relief plan further, consider combining these dietary adjustments with other strategies. Chiropractic care, such as posture-focused treatments available in Bondi Junction, can support spinal and nervous system health. Low-impact exercises and stress management techniques also complement this approach. If you’re in Bondi Junction, Dr Steve offers gentle, nervous-system-oriented chiropractic adjustments that could work well alongside your dietary efforts.
Disclaimer and Professional Guidance
Before making any big changes to your diet or lifestyle, it’s important to consult a healthcare professional, especially if you have pre-existing conditions or take medications. For example, anti-inflammatory foods like leafy greens or turmeric can sometimes interact with blood-thinning medications. A dietitian can help tailor a plan to your needs, guide you through reading food labels, and ensure you’re meeting your nutritional requirements. In Australia, you may even be able to claim rebates for dietitian services through Medicare or private health insurance, making expert advice more accessible.
This information is intended as general guidance and should not replace professional medical advice. Chiropractic care focuses on musculoskeletal health, and results can vary between individuals. Always consult a qualified healthcare professional before making any health-related decisions.
FAQs
Which foods might trigger pain flare-ups?
Certain foods might aggravate pain flare-ups, particularly those associated with increased inflammation. Examples include processed foods, refined sugars, and items rich in saturated fats. These types of foods can heighten inflammation in the body, potentially making pain more intense or harder to manage.
How long does an anti-inflammatory diet take to help with pain?
The effects of an anti-inflammatory diet on pain relief often take time to become noticeable – sometimes several weeks or even months. This is because the diet works by gradually lowering inflammation in the body. How quickly someone experiences results can depend on factors such as how consistently they follow the diet and their overall health condition.
Do I need supplements for omega-3, magnesium or vitamin D?
Supplements like omega-3, magnesium, or vitamin D might play a role in supporting overall health and managing inflammation. However, whether you need them depends on your individual circumstances. It’s always a good idea to consult with a healthcare professional who can assess your specific needs and guide you on the right approach.