Myofascial release therapy can help with muscle and fascia issues, but it’s not suitable for everyone. Using this therapy without proper screening can lead to serious complications. Here’s what you need to know:
- Avoid in certain conditions: Active cancer, infections, aneurysms, deep vein thrombosis (DVT), and uncontrolled hypertension.
- Use caution: Recent fractures, post-surgery areas, severe osteoporosis, or if on blood-thinning medication.
- Risks include: Bruising, internal bleeding, nerve damage, or worsening of existing conditions.
- Safety measures: Always review medical history, monitor symptoms during sessions, and seek medical clearance when necessary.
Knowing when not to use this therapy is essential for safe and effective care. Always consult a qualified professional for advice.
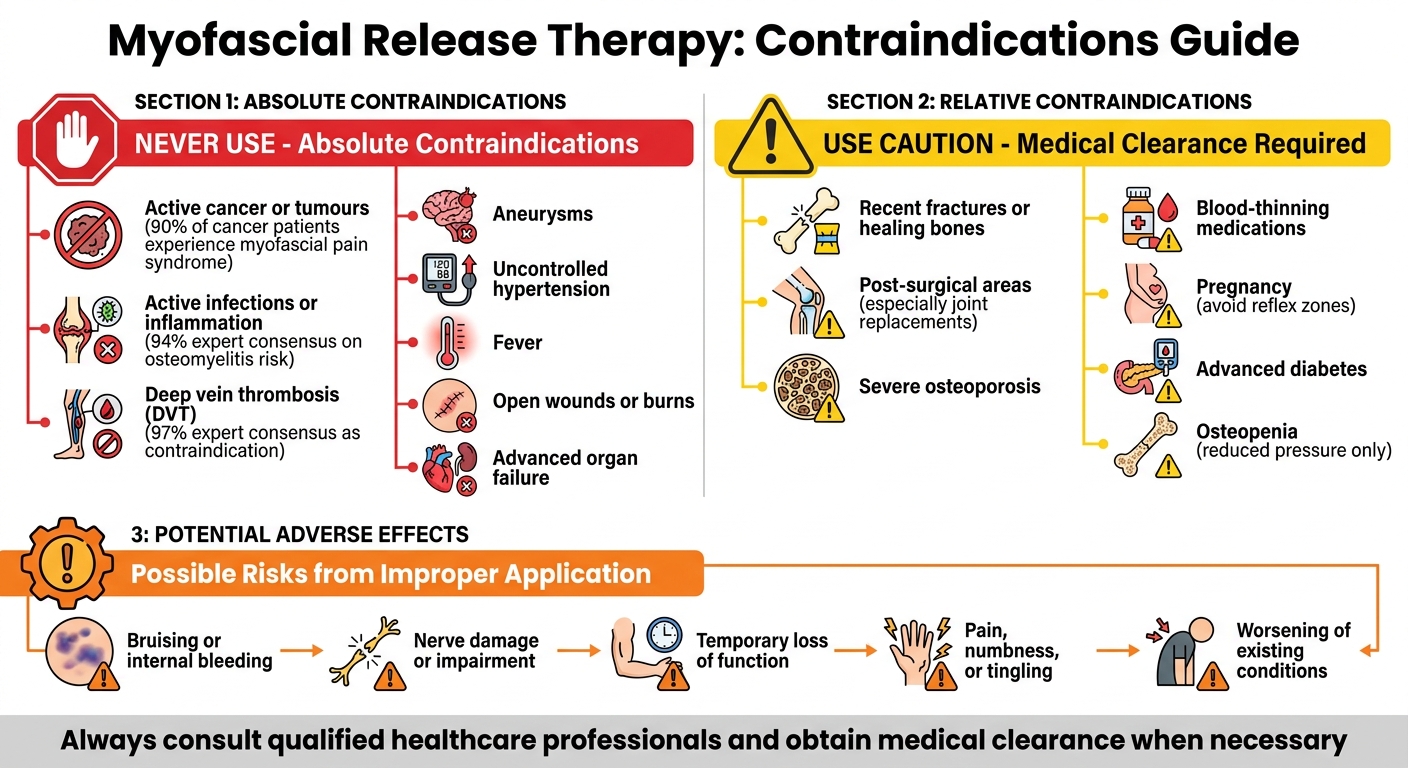
Myofascial Release Therapy Contraindications Guide
Question 15 of 21: What contraindications are there for carrying out myofascial release?
sbb-itb-585d67d
When Myofascial Release Should Never Be Used
There are specific situations where myofascial release therapy is not safe and can lead to serious complications. A detailed review of a patient’s medical history is essential to identify these risks. Below are the conditions where this therapy is strictly off-limits.
Cancer and Tumours
For patients with active cancer, myofascial release is not recommended. Applying pressure to areas affected by cancer or tumours can pose two major risks: it may spread cancer cells to other parts of the body or worsen tumour growth. As PalmLeaf Massage and Wellness explains:
"Manipulating tissue can risk spreading cancer cells."
This risk is especially concerning in cases of bone metastasis, where bones are already fragile and prone to damage. Studies show that up to 90% of cancer patients experience myofascial pain syndrome, with a prevalence ranging from 11.9% to 44.8% in those with cancers of the neck, head, or breast. This overlap highlights the need for careful screening to differentiate muscle pain from pain caused by bone metastases, which may require immobilisation rather than treatment.
It is essential to get medical clearance from an oncologist before considering myofascial release for anyone with a history of cancer. Under no circumstances should direct pressure be applied to tumour sites.
Active Infections or Inflammation
If a patient has an acute infection or inflammation, myofascial release should be avoided. Conditions such as cellulitis (a skin infection) or osteomyelitis (a bone infection) could worsen due to increased local spread. An expert panel reached a 94% consensus that osteomyelitis presents a significant risk due to the potential for severe complications.
Acute inflammation is part of the body’s healing process, and applying myofascial release during this time can interfere with recovery and even cause additional tissue damage. A fever is an absolute contraindication, as it signals the body is already under stress from fighting an infection. Similarly, open wounds, burns, or unhealed surgical incisions should not be treated, as increased blood flow could aggravate these conditions. Therapy should only be considered once all signs of acute inflammation have resolved, and the patient’s condition has stabilised.
Unstable Medical Conditions
Certain serious medical conditions make myofascial release unsafe. For example, individuals with aneurysms or deep vein thrombosis (DVT) face significant risks, as the therapy could lead to rupture or dislodge a clot, potentially causing life-threatening complications like a pulmonary embolism, stroke, or heart attack. Experts reached a 97% consensus that DVT should be treated as a clear contraindication for this therapy.
Uncontrolled hypertension is another concern, as the physical stress of treatment could cause a dangerous spike in blood pressure or trigger a cardiovascular event. Other conditions that require complete avoidance include advanced liver or kidney disease, organ failure, and uncontrolled seizure disorders. These conditions indicate a level of systemic instability that makes manual therapy too risky. A thorough medical history review is critical to identify these red flags before proceeding with any treatment.
Conditions Requiring Caution or Medical Clearance
While some situations completely rule out myofascial release therapy, others call for careful adjustments and medical clearance before proceeding. Here’s what you need to know.
Recent Fractures and Post-Surgical Areas
Fractures that are still healing or joints that are recently injured or unstable should not undergo myofascial release therapy. Applying pressure in these cases could interfere with recovery, risking re-injury or further instability.
For those who have had joint replacement surgery and completed rehabilitation, it’s crucial to consult the surgeon before restarting myofascial release. This ensures the surgical site has healed enough and that manual therapy won’t affect the repair. A detailed medical history review is key to identifying these cases and planning safe treatment.
Severe Osteoporosis or Weakened Bones
Severe osteoporosis makes bones highly fragile, making myofascial release unsuitable. For individuals with osteopenia, therapy might be possible but only with reduced pressure and medical clearance. Direct pressure on bony areas like the spine, knees, or elbows should be avoided entirely. Instead, focus on the surrounding muscles and fascia, keeping a close eye on the patient’s comfort. If any discomfort arises, adjust the pressure immediately.
Blood Clots and Vascular Problems
Deep vein thrombosis (DVT) is a strict no-go for myofascial release. Symptoms like redness, pain, swelling, numbness, or warmth in a specific area could signal a clot, and the patient should seek emergency care instead of manual therapy.
For those on blood-thinning medications, gentle pressure is a must, and medical clearance is non-negotiable. Be extra careful when working near major superficial blood vessels, such as in the neck or behind the knee. Always monitor the skin for any unusual reactions and modify techniques to prioritise safety.
Possible Adverse Effects
While myofascial release therapy is generally considered safe when performed by a skilled practitioner, improper application can lead to adverse effects. Understanding these risks is crucial for both practitioners and patients, ensuring informed decisions and better outcomes through thorough screening and assessment.
Bruising and Internal Bleeding
Applying too much pressure or using improper techniques can result in bruising or internal bleeding. This is particularly concerning for patients on blood-thinning medications or those with clotting disorders. Areas like the neck, abdomen, and the back of the knee are especially sensitive.
To avoid these issues, practitioners must carefully monitor for signs like discolouration, swelling, or discomfort. Adjusting pressure immediately when these signs appear is critical. Additionally, excessive force near nerve pathways can create further complications, making proper technique and pressure control essential.
Nerve Damage or Temporary Loss of Function
Applying excessive force near nerve pathways can lead to temporary or even permanent nerve impairment. Areas such as the neck, cervical spine, major joints, and regions where nerves are close to the surface require extra caution.
Patients may experience pain, numbness, or tingling – symptoms that should never be ignored. If these occur, practitioners must immediately adjust their technique to prevent further harm. A strong understanding of anatomy and careful application of pressure are key to reducing these risks.
Safety Guidelines and Screening Procedures
Safe myofascial release therapy relies on careful screening and collaboration, especially when contraindications are identified. A detailed initial assessment is critical, starting with a review of the patient’s medical history to identify absolute contraindications. This step builds on earlier risk assessments and highlights cautionary factors like pregnancy, anticoagulant use, or advanced diabetes. These conditions often require medical clearance or adjustments to the therapy plan.
Physical assessments should focus on identifying sensitive anatomical areas, such as those near major blood vessels, nerves, or vital organs. Specific regions like the neck, abdomen, and the back of the knee demand extra care. Practitioners should also monitor systemic factors, such as blood pressure, during evaluations. For individuals with osteopenia or osteoporosis, only minimal pressure should be applied to avoid fractures. This thorough screening process ensures therapy is both safe and tailored to the individual’s needs.
Medical History Review and Physical Assessment
The screening process must include checks for recent injuries, such as unhealed fractures, open wounds, or recent surgical incisions. It’s also essential to assess systemic stability by looking for signs of organ failure, fever, or cardiovascular issues. For patients on anticoagulant medications, consulting their physician is crucial. Techniques should then be adjusted to use gentler pressure, minimising the risk of bruising or internal bleeding.
Monitoring symptoms throughout the session is essential. Practitioners should be alert to sharp pain or numbness and adjust their approach immediately. Pregnant patients require special considerations, avoiding reflex zones like the soles of the feet, inner thighs, and calves. Consulting with a physician is particularly important during sensitive stages of pregnancy.
Working with Healthcare Professionals
Collaboration with other healthcare providers enhances safety, especially for patients with complex medical histories. For instance, patients who have undergone joint replacements should consult their surgeon to determine the appropriate timing and intensity for resuming therapy.
| Condition | Professional to Consult | Recommended Action |
|---|---|---|
| Joint Replacement (Post-Rehab) | Attending Surgeon | Determine timing for resuming therapy; assess risks |
| Anticoagulant Therapy | Physician | Use reduced pressure; monitor for bruising |
| Uncontrolled Hypertension | Physician | Monitor blood pressure; ensure stability |
| Advanced Diabetes | Physician | Check tissue health; apply lighter techniques |
| Pregnancy | Physician/Obstetrician | Avoid sensitive areas; reduce pressure |
Patient Education and Informed Consent
Clear communication about potential risks is a must. Practitioners should explain that temporary bruising or heightened sensitivity might occur and ensure patients fully understand the therapy before proceeding. Special care is needed for individuals with high anxiety or poorly managed psychiatric conditions to ensure their comfort and gain explicit consent.
Patients should also be educated about areas of the body that require extra caution, often referred to as "no-go zones." They need to know the importance of reporting sharp pain or numbness immediately, as these symptoms indicate the need to stop or modify the technique. Additionally, since fascia is interconnected, patients should understand that work in one area may have effects elsewhere in the body. This helps them grasp why the therapist might focus on regions distant from their primary site of pain.
Conclusion
Ensuring patient safety hinges on identifying contraindications, as we’ve explored in detail. Research highlights numerous contraindications tied to the circulatory, musculoskeletal, and integumentary systems. Without proper screening, complications such as dislodged clots, the spread of malignant cells, or vascular rupture can occur.
A thorough initial assessment, coupled with collaboration with healthcare professionals, forms the foundation of safe practice. For conditions requiring medical clearance – like anticoagulant therapy, recent joint replacements, or uncontrolled hypertension – seeking input from a physician ensures that treatment plans are aligned with patient needs while minimising risks. Additionally, real-time monitoring during sessions allows practitioners to adjust techniques promptly if symptoms like sharp pain or numbness arise.
Patient education is equally important. By informing patients about caution areas and warning signs, they can actively participate in maintaining their safety. The RECOVER Injury Research Centre at the University of Queensland advises practitioners to conduct detailed assessments and tailor treatments accordingly, while continuously monitoring the patient’s response and making necessary adjustments.
By combining thorough assessments, open communication, and patient involvement, practitioners can effectively manage risks while promoting musculoskeletal health.
This information is general in nature and does not replace professional medical advice.
Chiropractic care focuses on musculoskeletal health, and results can vary between individuals.
Please consult a qualified healthcare professional before making decisions about your health.
FAQs
How do I know if I’m safe for myofascial release?
Myofascial release therapy is typically safe for most people, but there are some conditions where it might not be suitable. These include recent fractures, malignancy, aneurysm, acute rheumatoid arthritis, advanced diabetes, or severe osteoporosis. These conditions could pose additional risks during treatment. It’s always best to consult a qualified healthcare professional to figure out if this therapy is the right choice for your situation.
What symptoms mean I should stop a session straight away?
You should end a myofascial release session right away if you feel pain, numbness, tingling, or any increase in discomfort. These sensations could mean that delicate areas like major blood vessels, nerves, or organs are being impacted, which could lead to harm if not addressed.
What should I tell my GP or surgeon before getting myofascial release?
Before beginning myofascial release therapy, make sure to discuss any potential contraindications with your GP or surgeon. These could include recent surgeries, fractures, or chronic conditions like malignancy, aneurysm, acute rheumatoid arthritis, advanced diabetes, or severe osteoporosis. Providing this information helps ensure the therapy aligns with your specific health requirements and is safe for you.