Chronic pain affects millions globally, with 1 in 5 people experiencing it, and 24% of U.S. adults reporting ongoing issues by 2023. Unlike acute pain, chronic pain persists beyond normal healing, often due to changes in the nervous system. These changes can amplify pain signals, causing symptoms like hyperalgesia (heightened pain response) and allodynia (pain from non-painful stimuli).
Key points:
- Chronic pain stems from nervous system dysfunction, including central sensitisation, where pain signals are exaggerated.
- Neurotransmitters like glutamate and reduced pain-inhibiting pathways worsen the condition.
- Brain changes, such as reduced grey matter volume in areas like the anterior cingulate cortex, further complicate pain perception.
- Stress, poor posture, and environmental triggers can intensify symptoms.
Treatment options include:
- Chiropractic care: Spinal adjustments may reduce nerve pressure and improve nervous system balance.
- Lifestyle changes: Correcting posture, ergonomic adjustments, and gentle exercises like yoga or walking can help.
- Stress management: Techniques like deep breathing and mindfulness may lower pain sensitivity.
Combining chiropractic care with movement strategies and stress reduction offers a multi-faceted approach to managing chronic pain. Always consult a healthcare professional for personalised advice.
The Neurobiology of Chronic Pain: Understanding a Stuck Alarm System
sbb-itb-585d67d
Central Sensitisation and Nervous System Dysfunction
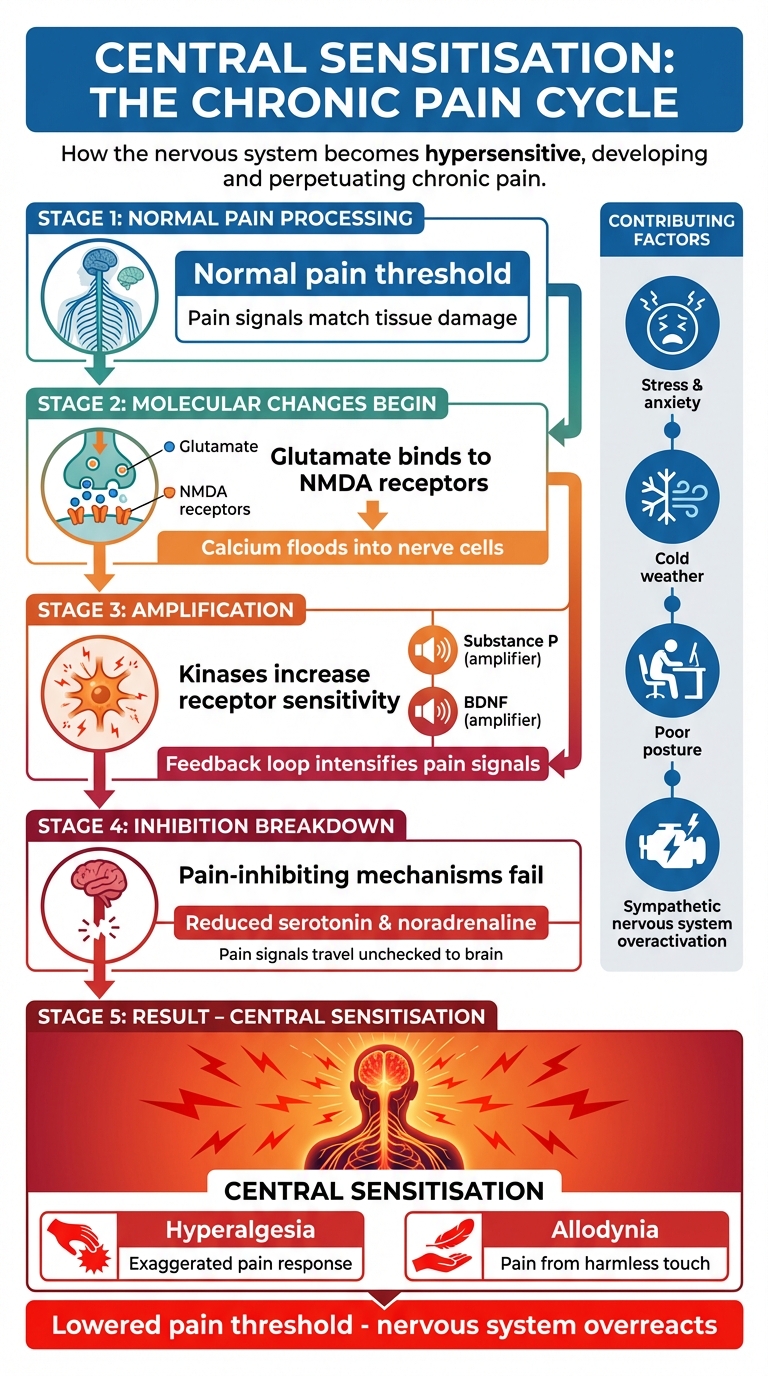
How Central Sensitisation Causes Chronic Pain in the Nervous System
How Central Sensitisation Works
Central sensitisation happens when the nervous system becomes overly sensitive, amplifying pain signals far beyond what the actual tissue damage would justify. This heightened sensitivity stems from molecular changes in the dorsal horn, the part of the spinal cord that processes pain signals.
A key player in this process is the neurotransmitter glutamate. When glutamate binds to NMDA receptors in the spinal cord, it causes calcium to flood into nerve cells. This calcium influx activates kinases, which increase the sensitivity of these receptors. Compounding the issue, substances like Substance P and brain-derived neurotrophic factor (BDNF) intensify this state of heightened sensitivity, creating a feedback loop that makes pain perception worse over time.
"Central sensitization is characterized as the enhancement in the function of neurons and circuits in nociceptive pathways caused by increases in membrane excitability and synaptic efficacy as well as to reduced inhibition and is a manifestation of the remarkable plasticity of the somatosensory nervous system…" – Marcin Karcz et al., Journal of Pain Research
Another critical aspect is the disruption of the body’s pain-inhibiting mechanisms. Normally, descending pathways from the brain release serotonin and noradrenaline to dampen pain signals at the spinal cord level. In chronic pain conditions, these pathways can weaken or malfunction, allowing pain signals to travel unchecked to the brain. Studies have found that individuals with conditions like fibromyalgia often show reduced levels of serotonin and noradrenaline in their bodily fluids compared to those without chronic pain.
These changes at the molecular and cellular levels lower the nervous system’s pain threshold, which significantly alters how pain is perceived.
Changes in Pain Perception
Central sensitisation doesn’t just amplify pain; it changes how the body processes sensory information altogether. Two major effects are hyperalgesia and allodynia. Hyperalgesia refers to an exaggerated response to pain – something mildly painful feels far more intense. Allodynia, on the other hand, is when normally harmless sensations, like a light touch or the pressure of clothing, are interpreted as painful.
This happens because the nervous system lowers its threshold for triggering pain signals. Both fast and slow pain fibres become hypersensitive, and even sensory fibres that don’t usually carry pain signals can start sending pain messages.
Environmental factors like cold weather, stress, or anxiety can further worsen pain in people with central sensitisation. This is tied to the over-activation of the sympathetic nervous system, which governs the "fight or flight" response. Elevated levels of norepinephrine and epinephrine fuel the production of pro-inflammatory cytokines. These inflammatory substances can cause harmful changes in the brain, perpetuating the cycle of pain sensitivity.
Brain Changes Associated with Chronic Pain
Physical Changes in Brain Structure
Chronic pain doesn’t just influence how you feel – it can actually reshape your brain. Studies reveal that people enduring ongoing pain often show reduced grey matter volume in specific brain areas. The most affected regions include the anterior cingulate cortex (ACC), which processes the emotional aspects of pain, the insula, responsible for sensory awareness and interpreting bodily signals, and the prefrontal cortex, which handles decision-making and emotional control.
These changes are driven by neuroplasticity, the brain’s ability to adapt and reorganise. While neuroplasticity usually helps us learn and adjust, in the case of chronic pain, it can backfire. The brain essentially "over-learns" pain, reinforcing pathways that keep the sensation alive, even if the original injury has healed.
A key factor in these structural changes is a drop in proteins called neurotrophins, particularly brain-derived neurotrophic factor (BDNF) and nerve growth factor (NGF). These proteins are vital for neuron health and maintaining connections between brain cells. When their levels decline, the brain struggles to regulate pain and mood. This may help explain why depression affects between 50% and 65% of people living with chronic pain.
Structural changes are only part of the story – chronic pain also alters how different brain regions interact.
Disrupted Brain Network Function
Chronic pain doesn’t just alter brain structure; it also disrupts communication between brain networks. The brain relies on interconnected systems to process pain and manage emotional responses. However, persistent pain can throw these systems into disarray. Areas like the anterior insular cortex, inferior frontal gyrus, bilateral anterior cingulate cortex, and orbitofrontal cortex – all involved in processing pain and emotions – are particularly affected.
One major disruption occurs in the autonomic nervous system, which becomes imbalanced. The sympathetic nervous system (responsible for the "fight or flight" response) becomes overactive, while the parasympathetic system (the "rest and digest" mode) is suppressed. This imbalance keeps the body in a heightened state of alertness, lowering the threshold for pain. As Dr. Nicholas Miller from Healthspace Clinics notes:
"When your system is amped, your threshold for pain drops."
This heightened state triggers a chain reaction of neurochemical changes. Increased levels of norepinephrine and epinephrine lead to the production of pro-inflammatory cytokines, which can cause neuroinflammation and damage brain cells. These changes also disrupt neurotransmitters like serotonin and noradrenaline, creating a vicious cycle that fuels both pain and mood disorders. The thalamus, the brain’s relay centre for pain signals, plays a central role here, influencing both the intensity of pain and its emotional impact.
How Chiropractic Care May Help Manage Chronic Pain
Spinal Adjustments and Nervous System Function
Chiropractic adjustments aim to realign spinal joints, which can help reduce nerve pressure and ease muscle tension – two factors often linked to chronic pain. When spinal joints aren’t moving properly, they can contribute to inflammation, creating a cycle that perpetuates discomfort.
There’s some evidence suggesting that spinal manipulation may influence the autonomic nervous system. For example, adjustments to the cervical spine often trigger a parasympathetic response, which may help lower heart rate and blood pressure. Meanwhile, adjustments to the thoracic and lumbar regions tend to activate the sympathetic system. This ability to influence nervous system activity could help correct imbalances that are associated with chronic pain.
Research has also shown that spinal adjustments may encourage the release of neurotrophins like BDNF (brain-derived neurotrophic factor) and NGF (nerve growth factor). These substances play a role in maintaining neuronal health and adaptability, potentially improving the nervous system’s ability to regulate pain signals. While further studies are needed, these findings highlight a possible connection between chiropractic care and pain management.
"The kinds of chronic pain most effectively treated with chiropractic care are joint related…neck, back, hips, shoulders. Chiropractic care will loosen up the muscles in that area…and help mobilise those joints and allow those joints to function in the way they’re meant to function."
- Dr. Jeremy Coffey, Chiropractor, Western Reserve Hospital
Addressing Posture and Movement Problems
Beyond spinal adjustments, chiropractors often focus on correcting posture and movement issues that can exacerbate chronic pain. Poor posture, especially for those who spend long hours at a desk, can place undue strain on the spine and surrounding muscles. This can lead to persistent pain in the neck, shoulders, and back.
Chiropractic care may help by realigning the spine and addressing these postural stressors, which could reduce nerve irritation and improve nervous system function. Techniques like joint mobilisation, myofascial release, and postural training are often used to target the soft tissues contributing to chronic pain. For office workers, ergonomic recommendations can help alleviate conditions like tech-neck and tension headaches. Chiropractors may also suggest simple stretches or low-impact exercises, such as yoga or walking, to strengthen spinal support muscles and improve overall movement.
Working Alongside Other Treatments
Chiropractic care tends to be most effective when combined with other chronic pain management strategies. Chiropractors often work alongside physiotherapists, exercise physiologists, and other healthcare professionals to provide well-rounded care. For example, while chiropractic adjustments may improve joint mobility and reduce nerve irritation, physiotherapy can focus on strengthening core muscles and improving posture for long-term relief.
Stress management techniques, like deep breathing exercises, may also complement chiropractic care by helping to regulate autonomic function and reduce tension. Low-impact activities, such as swimming or walking, can further aid recovery by improving circulation and encouraging the release of natural endorphins.
"We can go down parallel paths toward the same goal [of improving quality of life by eliminating chronic pain]."
- Dr. Jeremy Coffey, Chiropractor, Western Reserve Hospital
By combining chiropractic care with other treatments and lifestyle changes, individuals may find a more comprehensive approach to managing chronic pain.
This information is general in nature and is not a substitute for professional medical advice.
Chiropractic care focuses on musculoskeletal health and results vary between individuals.
Please consult a qualified healthcare professional before making decisions about your health.
Lifestyle and Movement Strategies for Chronic Pain
Chiropractic adjustments are just one piece of the puzzle when it comes to managing chronic pain. Incorporating simple lifestyle changes into your daily routine can further support your nervous system and improve musculoskeletal health.
Improving Ergonomics and Posture
If you spend long hours at a desk, making ergonomic adjustments could make a big difference in managing chronic pain. Small tweaks – like raising your chair to the right height, positioning your screen at eye level, or adding a lumbar cushion – can help realign your spine and ease nerve pressure. These adjustments may address common sources of joint discomfort, especially in the neck and back.
Pairing postural training with core-strengthening exercises is another effective way to stabilise your spine. Stronger core muscles help reduce strain on your joints, offering long-term support. Combined with spinal adjustments, these strategies can help you navigate daily physical stresses more comfortably. Many chiropractors and healthcare professionals often recommend these approaches as part of a broader plan to manage chronic pain.
Exercise and Movement for Pain Relief
Engaging in low-impact activities like walking, swimming, or yoga can improve flexibility and circulation without putting too much stress on sensitive joints. Research highlights the benefits of combining manual therapies with movement-based strategies for addressing chronic neck and back pain. Start with gentle exercises and gradually increase intensity as your body adjusts.
Incorporating range-of-motion exercises into your routine can also help combat stiffness, a common issue for those with chronic pain. Regular movement promotes better blood flow and helps flush out inflammatory substances from affected areas. For a more personalised approach, some people track their Heart Rate Variability (HRV) to monitor how their nervous system responds to lifestyle changes and stress management efforts.
Managing Stress and Tension
Chronic pain often intertwines with mood and sleep issues, all connected through the nervous system. Stress management techniques – like deep breathing, mindfulness, or gentle stretching – can help lower the body’s pain response.
Identifying and managing environmental triggers, such as cold weather or high-stress situations, may also help reduce pain flare-ups. Complementary therapies like massage or aromatherapy can further calm the nervous system and reduce sensitivity. The ultimate aim is to retrain your nervous system to process sensations without triggering pain, giving you more control over your daily life.
Conclusion
Chronic pain often stems from an imbalance in the nervous system, involving mechanisms like central sensitisation and changes in brain networks. Central sensitisation, in particular, makes the nervous system overly sensitive, causing even harmless stimuli to feel painful. Studies indicate that around 1 in 4 Australian adults live with chronic pain, and nearly 1 in 10 report that it disrupts their daily lives significantly.
Addressing this dysfunction calls for a comprehensive approach. Chiropractic care may play a role in supporting nervous system health through spinal adjustments that target joint issues and nerve interference. When paired with lifestyle changes – like improving ergonomics, engaging in gentle physical activity, and practising stress management – these methods can work together to help regulate nerve responses and restore balance.
Through manual therapies, movement strategies, and stress reduction, these approaches aim to recalibrate the nervous system. If persistent musculoskeletal pain is affecting your life, consider seeking personalised care from qualified professionals. For those in need, Chiropractor Bondi Junction offers care focused on nervous system health to support overall musculoskeletal wellbeing. This integrated approach combines evidence-based chiropractic care with practical lifestyle adjustments to address chronic pain.
This content is for general informational purposes and should not replace professional medical advice. Chiropractic care focuses on musculoskeletal health, and outcomes may vary. Always consult a qualified healthcare provider before making health-related decisions.
FAQs
How can I tell if my pain is due to central sensitisation?
Central sensitisation happens when the nervous system becomes overly reactive, making pain signals feel more intense than they should. This can show up as widespread pain, an exaggerated response to things that wouldn’t normally hurt (like a light touch), or pain that sticks around long after an injury has healed. Other possible symptoms include fatigue and a general increase in sensitivity. Diagnosing this condition requires a thorough evaluation by a healthcare professional. If you’re dealing with ongoing or unexplained pain, it’s important to reach out to a qualified provider to explore potential causes and treatment options.
Can chronic pain occur even after an injury has healed?
Chronic pain can continue even after an injury has fully healed. Studies indicate this may be due to dysfunction in the nervous system and alterations in brain pathways. These changes can cause the pain to persist, functioning independently of any ongoing tissue damage.
Is chiropractic care suitable for my type of chronic pain?
Chiropractic care is often considered as an option for managing specific types of chronic pain, particularly those related to nerve or musculoskeletal problems. By focusing on spinal adjustments, chiropractors aim to improve spinal alignment, which can help minimise nerve interference. This improved alignment may enhance communication between the brain and the rest of the body, potentially supporting the body’s natural ability to heal itself. For conditions such as herniated discs or sciatica, this approach might offer some relief. Always consult a qualified healthcare professional to see if chiropractic care is appropriate for your particular situation.