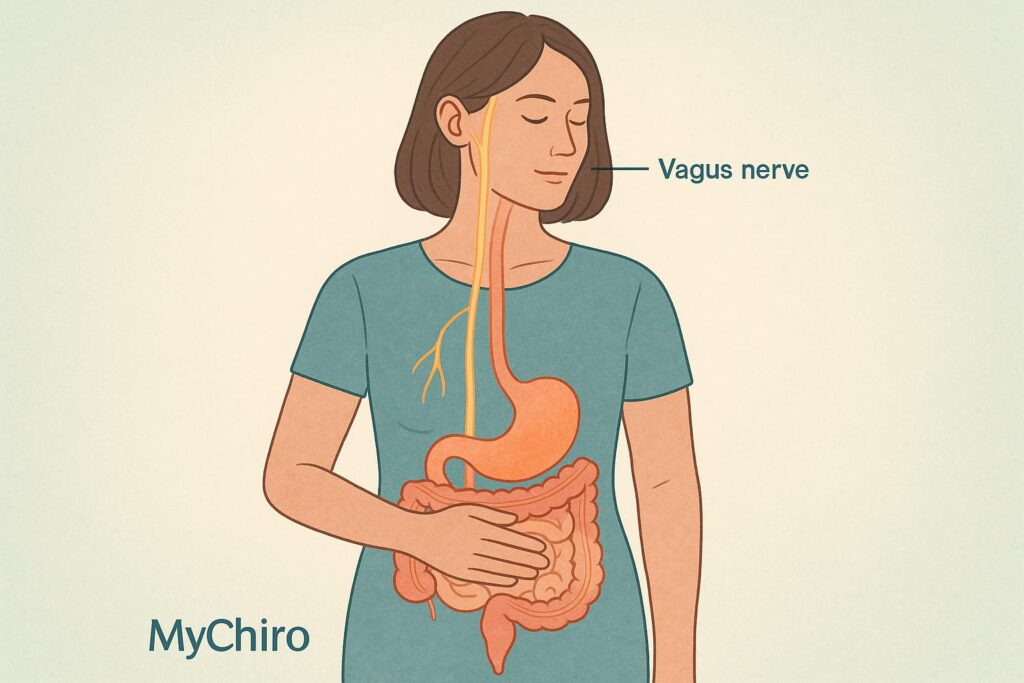
Acid reflux isn’t always caused by too much stomach acid. It can also result from issues with the vagus nerve, which plays a key role in digestion. This nerve helps control stomach acid production, food movement, and the lower oesophageal sphincter (which prevents acid from flowing back into the oesophagus). When the vagus nerve isn’t working properly, digestion slows down, pressure builds in the stomach, and reflux symptoms can worsen.
Key takeaways:
- The vagus nerve connects the brain to the digestive system, managing essential functions like acid production and food movement.
- Poor vagus nerve function can lead to symptoms like heartburn, bloating, and delayed stomach emptying.
- Stress, poor posture, and spinal misalignments may interfere with vagus nerve signalling.
- Chiropractic care and lifestyle changes – like improving posture, practising stress management, and using breathing techniques – may help support vagus nerve activity and ease reflux symptoms.
This article explores how the vagus nerve affects digestion, the connection to acid reflux, and practical steps to improve nerve health and reduce discomfort.
Digestion & the Vagus Nerve: Sphincter function and related symptoms affected by neck instability
The Vagus Nerve’s Role in Digestion
The vagus nerve plays a crucial role in digestion through its intricate network of neurons, which work closely with the enteric nervous system. Together, they ensure the digestive process runs smoothly and efficiently.
When everything is working as it should, the vagus nerve helps stimulate stomach acid production, controls the pyloric valve, coordinates the release of bile and digestive enzymes, and maintains the rhythmic contractions of the digestive tract.
But the vagus nerve isn’t just about digestion. It’s a key player in the parasympathetic nervous system – often called the "rest and digest" system. When this system is active, it creates the ideal conditions for digestion by slowing the heart rate, boosting digestive secretions, and improving gut motility. On the flip side, when the sympathetic nervous system (commonly linked to stress) dominates for too long, it can interfere with these processes and potentially lead to digestive issues.
Interestingly, research indicates the vagus nerve also helps regulate inflammation, influencing organs like the spleen and liver. This connection adds another layer to its impact on digestive health.
How Vagus Nerve Problems Affect Acid Reflux
When the vagus nerve isn’t functioning properly, it can disrupt stomach acid production and delay the emptying of the stomach. This can increase stomach pressure, raising the likelihood of acid reflux. Improper digestion may also lead to fermentation, which produces gas and further heightens stomach pressure, triggering reflux episodes.
A poorly functioning vagus nerve can also weaken the lower oesophageal sphincter and slow oesophageal motility. This means acid may linger in the oesophagus longer, causing discomfort.
In some cases, vagus nerve dysfunction can cause broader symptoms like chest pain, dizziness, fainting, or irregular heart rhythms. These issues often go hand-in-hand with digestive symptoms, creating a complex web of discomfort.
Common Signs of Vagus Nerve Problems
Problems with the vagus nerve often show up as digestive troubles, such as acid reflux, heartburn, bloating, and other related issues.
When vagal coordination is impaired, symptoms like gas, bloating, difficulty swallowing, irregular bowel movements, and even fatigue or food sensitivities can emerge. These issues highlight the potential advantages of therapies that support both spinal health and nervous system function.
In more severe cases, vagus nerve dysfunction may lead to gastroparesis – a condition where the stomach empties too slowly. This can cause nausea, vomiting, early feelings of fullness, and general discomfort, often made worse by stress, exhaustion, or poor posture.
How Chiropractic Care May Support Nervous System Function
Chiropractic care often focuses on the relationship between spinal health and the nervous system. One key connection is the vagus nerve, which plays a critical role in regulating digestion. It’s thought that spinal alignment and overall nervous system balance may influence how effectively the vagus nerve functions.
By addressing spinal alignment, chiropractic care may help promote a more balanced nervous system. Chiropractic adjustments aim to correct spinal misalignments, which may encourage the body to shift into a parasympathetic state – commonly referred to as the "rest and digest" mode. However, it’s important to understand that chiropractic care primarily targets musculoskeletal health, and any impact on digestive function is considered indirect. It’s not a direct treatment for conditions like acid reflux.
Conventional treatments for acid reflux often focus on lowering stomach acid with medications. Some practitioners, however, suggest that improving spinal alignment could indirectly support digestive health by optimising vagus nerve function.
How Spinal Adjustments May Help
The vagus nerve extends from the brainstem, through the neck and chest, and into the abdomen. Misalignments in the spine, particularly in the cervical (neck) area, can compress or irritate the nerve pathways that are important for vagus nerve signalling.
Research indicates that instability in the cervical spine may impact vagus nerve performance. Chiropractic adjustments targeting the cervical and upper thoracic spine aim to restore alignment and reduce nerve compression. These adjustments may improve spinal mobility and support the nervous system as a whole.
In fact, a 2020 systematic review highlighted that spinal manipulation might positively influence heart rate variability – a marker linked to the autonomic nervous system and vagus nerve activity [1].
The goal of these adjustments isn’t just to alleviate pain. Rather, they aim to create conditions that allow the nervous system to better balance sympathetic (fight or flight) and parasympathetic (rest and digest) activity. When the body can more easily enter a relaxed state, the vagus nerve may be better equipped to support digestive processes. That said, these benefits are indirect. Beyond adjustments, posture also plays a significant role in nervous system function.
The Connection Between Posture and Digestive Symptoms
Posture affects more than just your neck and back – it can also influence how your nervous system operates. Poor posture, such as forward head positioning and rounded shoulders (common among desk workers), can lead to tension and misalignment in the cervical and thoracic spine. These issues may narrow the pathways the vagus nerve uses, potentially interfering with its ability to send signals effectively.
Chronic poor posture can also reinforce a state of stress within the nervous system. Since the vagus nerve is most active during relaxed, "rest and digest" states, constant postural stress may inhibit its activation. Spending hours hunched over a desk or phone creates tension patterns that signal stress, making it harder for the body to relax and function optimally.
Chiropractic care works to address these postural challenges by correcting spinal misalignments and reducing tension patterns. By improving spinal alignment, chiropractic adjustments may help break the cycle of stress-related signalling, indirectly contributing to overall wellbeing. Seeking advice from a qualified practitioner can be a valuable step in maintaining musculoskeletal and nervous system balance.
sbb-itb-585d67d
Lifestyle Changes to Support Vagus Nerve Health
Beyond spinal care, everyday habits can play a big role in supporting vagus nerve function and easing digestive discomfort. Reducing stress and tension is particularly important, as chronic stress can interfere with vagus nerve activity and contribute to digestive issues like acid reflux. Simple lifestyle adjustments can complement other treatments to promote nerve and digestive health.
Posture and Movement Tips
Maintaining good posture is essential for spinal alignment and healthy nerve function. Sitting upright – whether at your desk or during meals – can help minimise pressure on the vagus nerve and your digestive organs. This is especially relevant in Australia, where many people spend extended hours working at desks or using mobile devices.
Regular movement is just as important. Activities like taking a walk after meals, stretching, or breaking up long periods of sitting can improve nerve signalling and digestion. Moderate aerobic exercises may also enhance vagus nerve function and reduce episodes of reflux.
Incorporating simple postural exercises can further support nerve health. Gentle neck stretches, shoulder rolls, and exercises to improve thoracic spine mobility can relieve tension along the vagus nerve pathway. Techniques like chin tucks and side-to-side neck stretches can help ease cervical strain, which indirectly supports proper nerve signalling. Practices that blend movement with mindfulness – such as yoga or tai chi – can also encourage a shift from the "fight or flight" mode to the calming "rest and digest" state.
Stress Management and Breathing Techniques
Reducing stress is a vital part of supporting vagus nerve health. Chronic stress keeps your body stuck in "fight or flight" mode, which suppresses vagus nerve activity. Thankfully, there are easy, evidence-backed techniques to help your body transition into a calmer "rest and digest" state.
Diaphragmatic breathing is one such method. To try it, inhale slowly through your nose for a count of four, allowing your belly to rise, then exhale gently through your mouth for six to eight counts. Practising this for five to ten minutes a day can help activate the vagus nerve and promote relaxation.
Research also shows that slow, deep breathing – around six breaths per minute – can boost vagal tone, as seen in improved heart rate variability. This technique may help alleviate symptoms of acid reflux and anxiety and can be done almost anywhere: at your desk, during your commute, or before a meal.
Mindfulness practices like meditation, progressive muscle relaxation, and mindful eating can further enhance parasympathetic activity. Simple habits like eating slowly, chewing thoroughly, and minimising distractions during meals can improve digestive comfort. Even a quick mindfulness session or a few deep breaths before eating can prepare your body for digestion.
Combining movement with stress management can amplify these benefits. For instance, taking a gentle walk while practising deep breathing may be more effective for improving vagal tone and digestion than either activity alone.
This information is general and does not replace professional medical advice.
Chiropractic care focuses on musculoskeletal health, and results may vary.
Always consult a qualified healthcare professional before making health decisions.
Conclusion: A Complete Approach to Managing Acid Reflux
Managing acid reflux effectively means addressing both the digestive system and the nervous system. At the centre of this connection is the vagus nerve, which plays a key role in regulating digestion. When this nerve doesn’t function as it should, it can lead to issues like reduced stomach acid, delayed gastric emptying, and weakened digestive reflexes. These disruptions often manifest as symptoms such as heartburn, bloating, and regurgitation.
A well-rounded approach is more effective than relying on a single solution. Chiropractic care, for instance, may assist in improving nervous system function by addressing spinal misalignments, particularly in the cervical and upper thoracic spine. Dr Steve’s practice in Bondi Junction focuses on spinal and postural alignment, which may indirectly contribute to better digestive comfort.
Lifestyle changes are equally important in supporting vagus nerve health. Stress, fatigue, and anxiety can negatively impact vagal function, so incorporating daily practices like diaphragmatic breathing and mindfulness exercises can help activate the parasympathetic "rest and digest" state. Additionally, maintaining good posture – especially during long hours at a desk, as is common in many Australian workplaces – can reduce pressure on digestive organs and promote proper nerve signalling. These habits work hand-in-hand with professional care to improve overall well-being.
It’s vital to consult medical professionals for accurate diagnosis and treatment of underlying conditions. They can provide testing, prescribe medications when necessary, and rule out serious causes of reflux, ensuring your health is managed safely. Combining these medical insights with lifestyle adjustments and chiropractic care creates a balanced and effective approach.
Taking steps to address acid reflux doesn’t have to be complicated. A consultation with a chiropractor can help assess your spinal health and posture, particularly if you experience reflux alongside neck or back discomfort. Incorporating daily practices like diaphragmatic breathing and making ergonomic adjustments can complement professional care. By working with healthcare professionals, you can develop a personalised plan to support both immediate relief and long-term digestive health.
This information is general in nature and does not replace professional medical advice.
Chiropractic care focuses on musculoskeletal health, and results may vary between individuals.
Always consult a qualified healthcare professional before making decisions about your health.
FAQs
Could my acid reflux be linked to vagus nerve dysfunction rather than just excess stomach acid?
The relationship between acid reflux and the vagus nerve is intricate. While acid reflux is commonly linked to excess stomach acid, there’s some evidence suggesting that issues with the vagus nerve might also play a role. This nerve is crucial for regulating digestion, and disruptions in its function could potentially contribute to reflux symptoms.
If you think your acid reflux might be connected to vagus nerve dysfunction, it’s a good idea to speak with a qualified healthcare professional. In some cases, chiropractic care, which emphasises spinal and nervous system health, may help support vagus nerve function. However, keep in mind that results can vary from person to person, so discussing your specific symptoms with a practitioner is essential to determine suitable care options.
This information is provided as general guidance and should not replace professional medical advice. Chiropractic care primarily addresses musculoskeletal health, and outcomes differ between individuals. Always consult a qualified healthcare professional before making decisions about your health.
How can I support my vagus nerve health to help with acid reflux symptoms?
The vagus nerve has a fascinating and intricate role in digestion, and making certain lifestyle adjustments may help support its function, potentially easing symptoms of acid reflux. While chiropractic care primarily addresses musculoskeletal health, adopting specific habits can contribute to a balanced nervous system.
Here are a few changes to consider for supporting vagus nerve health:
- Manage stress: Incorporate practices like deep breathing, meditation, or yoga to help calm your nervous system.
- Eat mindfully: Avoid foods that trigger reflux and aim for a well-rounded, balanced diet.
- Stay active: Regular physical activity promotes overall health and can positively impact your nervous system.
- Prioritise quality sleep: Adequate rest allows your body to recover and perform at its best.
As always, it’s essential to consult a qualified healthcare professional to tailor these suggestions to your specific needs and ensure they’re right for your situation.
This is general information and not a replacement for professional medical advice. Chiropractic care focuses on musculoskeletal health, and outcomes can vary between individuals. Always seek guidance from a qualified healthcare professional before making health-related decisions.
Can chiropractic care help with acid reflux by supporting the vagus nerve?
Chiropractic care might influence the function of the vagus nerve, which is involved in regulating essential bodily processes like digestion. That said, it’s important to note that chiropractic care isn’t a direct remedy for acid reflux. Instead, it centres on improving musculoskeletal health and may indirectly support nervous system balance, potentially contributing to overall wellbeing.
Chiropractic adjustments are designed to enhance spinal alignment and optimise nervous system function. Some individuals find this approach helpful in managing stress and tension, which can sometimes aggravate symptoms. If you’re thinking about trying chiropractic care, it’s best to consult a qualified practitioner to determine if it aligns with your specific needs.
This information is intended for general purposes only and should not replace professional medical advice. Chiropractic care addresses musculoskeletal health, and outcomes can vary from person to person. Always seek guidance from a qualified healthcare professional before making decisions about your health.